SLIDE 1 5/23/2015 1 Small Glandular Proliferative Lesions of the Breast
Yunn-Yi Chen, MD, PhD Professor Director of Immunohistochemistry Laboratory Director of Breast Pathology Services UCSF Small Glandular Lesions of Breast
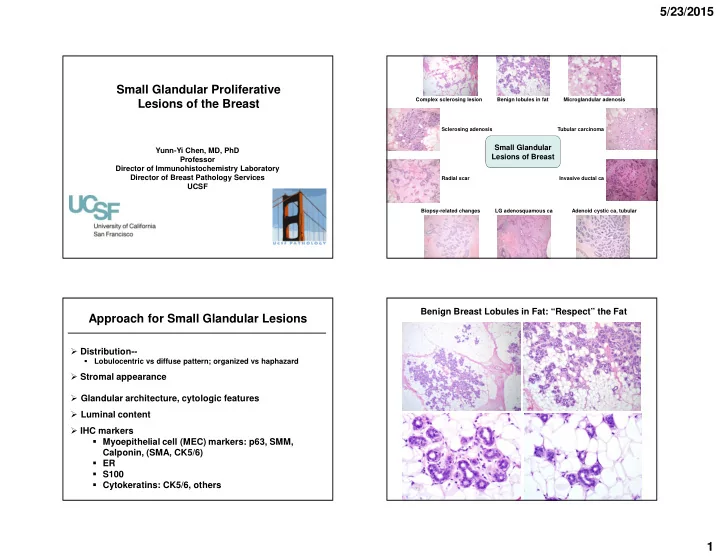
Complex sclerosing lesion Benign lobules in fat Microglandular adenosis Sclerosing adenosis Radial scar Tubular carcinoma Invasive ductal ca Biopsy-related changes LG adenosquamous ca Adenoid cystic ca, tubular
Distribution--
- Lobulocentric vs diffuse pattern; organized vs haphazard
Stromal appearance Glandular architecture, cytologic features Luminal content IHC markers Myoepithelial cell (MEC) markers: p63, SMM, Calponin, (SMA, CK5/6) ER S100 Cytokeratins: CK5/6, others
Approach for Small Glandular Lesions
Benign Breast Lobules in Fat: “Respect” the Fat

SLIDE 2
5/23/2015 2
Radial Sclerosing Lesion: “Respect” the Fat Invasive Ductal Carcinoma: Invade the Fat
Sclerosing Adenosis (SA)
Lobulocentric Stroma: collagenous, myxoid Glands and epithelial cells:
Glands compressed/central, open/peripheral; basement membrane Luminal epithelial and myoepithelial cells (MEC) Epithelial cells: flat to cuboidal, bland
Lumen: Calcifications IHC: Positive MEC markers

SLIDE 3
5/23/2015 3 Sclerosing Adenosis
Incidental or mammographic calcifications Mimic invasion Nodular adenosis Involved by lobular neoplasia or DCIS Apocrine cytology Perineural invasion
Nodular Adenosis
Florid sclerosing adenosis, nodular contour Mammographic mass or palpable lesion Also “adenosis tumor” (connotation of neoplasm)

SLIDE 4
5/23/2015 4
Biopsy for Mammographic Mass with Calcifications
Nodular adenosis
Sclerosing Adenosis and Nodular Adenosis
p63 CK5/6 SMM
Lobular Neoplasia Involving SA
Mimic invasive carcinoma Lobulocentric MEC markers
Apocrine Adenosis

SLIDE 5 5/23/2015 5 Apocrine Adenosis Apocrine Adenosis
SA with apocrine cytology
Eosinophic granular or foamy cytoplasm
Mimic carcinoma
Lobulocentric, MEC markers
Atypical apocrine adenosis
Invasive Apocrine CA Mimicking Apocrine Adenosis
SMM
Atypical Apocrine Adenosis--
3x nuclear enlargement with prominent pleomorphic nucleoli
(O’Malley FP and Bane AL. Adv Anat Pathol 2004)

SLIDE 6 5/23/2015 6 Apocrine Adenosis
SA with apocrine cytology
Eosinophic granular or foamy cytoplasm
Mimic carcinoma Atypical apocrine adenosis
3x nuclear enlargement, prominent pleomorphic nucleoli Long-term breast cancer risk: not well-defined On CNB: recommend excision to exclude DCIS On excision: regular follow-up
(Carter D et al: Mod Pathol 1991; Seidman J et al: Cancer 1996; Fuehrer N et al: Arch Pathol Lab Med 2012)
DCIS with Apocrine Features
p63
Sclerosing Adenosis with Perineural “Invasion” CNB for a Palpable Lesion

SLIDE 7
5/23/2015 7
p63 SMM
Sclerosing Lesion with Perineural “Invasion”
Peri- and Intraneural “Invasion” in Benign Breast Lesions
Ackerman: 1st description in 1957 Taylor and Norris (AFIP): series of 20 patients in 1967 Incidence: ~2% Also reported in benign lesions of other anatomic sites In breast: SA, radial scar, sclerosing papilloma Pathogenesis unclear : post-traumatic, involvement by the proliferative process
Radial Scar

SLIDE 8
5/23/2015 8 Radial Scar (RS)
Tumor-like or pseudoinfiltrative lesion Stellate appearance
Mimic malignancy on imaging and pathology
Central fibroelastotic core with entrapped distorted tubules, surrounded by radiating ducts and lobules Radiating ducts and lobules: variable changes (UDH, papillomatosis, adenosis, apocrine metaplasia, cysts)
Radial Scar
Radial Scar Invasive Ductal CA
RS: Fibroelastotic and Hypocellular Center with Entrapped Distorted Glands

SLIDE 9
5/23/2015 9
Entrapped Glands in Fibroelastotic Stroma
Distorted, compressed, angulated Luminal epithelial cells: flat to cuboidal Myoepithelial layer
Radiating Ducts and Lobules
Variable epithelial changes UDH, papillomatosis, adenosis, apocrine metaplasia, cysts
Radial Sclerosing Lesion (RSL)
Include radial scar and complex sclerosing lesion Radial scar: Smaller (≤ 1 cm) lesions, stellate Complex sclerosing lesion: larger lesions, more complex and extensive features
Complex Sclerosing Lesion

SLIDE 10 5/23/2015 10
Complex Sclerosing Lesion Attenuated Myoepithelial (MEC) Staining in RSL
SMM CK5/6 p63
Phenotypic Alterations in Myoepithelial Cells Associated with Sclerosing Lesions and DCIS
Expression of MEC markers: reduced or focally absent in various benign sclerosing lesions and DCIS Frequency:
SMM > p63, calponin > SMA Radial scar > sclerosing adensois
Panel of MEC markers Avoid over-diagnosis
When in doubt about the presence of invasion, diagnose as non-invasive
(Hilson JB et al: Am J Surg Pathol 2009 and 2010)
Radial Sclerosing Lesions
Organized Stroma: Fibroelastotic Glands and epithelial cells:
Distorted, compressed, angulated Luminal epithelial and myoepithelial cells (MEC) Epithelial cells: flat to cuboidal, bland
Lumen: Calcifications IHC: Positive MEC markers
Reduced or focally absent for MEC expression

SLIDE 11
5/23/2015 11
Tubular Carcinoma--
Diffuse/infiltrative growth
Tubular Carcinoma--
Desmoplastic or elastotic stroma
Tubular Carcinoma with FEA

SLIDE 12 5/23/2015 12
Infiltrative Desmoplastic cellular stroma, ± elastosis Open round, oval, or angulated tubules Cytology
- Single layer, non-stratified, cuboidal to columnar cells,
prominent cytoplasmic apical snouts
- Minimal pleomorphism, basally located round to oval nuclei
- Mitosis rare
Lack all MEC markers Diffusely and strongly positive for ER
Tubular Carcinoma
> 90% with tubular morphology Incompatible features--
- Complex architecture
- Multiple layers of cells
- Significant nuclear pleomorphism
- Frequent mitoses
Diagnosing Tubular Carcinoma
10-year survival: ~100% LN metastasis: rare, 1 node, no significant impact on survival Luminal A
- ER/PR +, HER2 -, low Ki-67
Tubular Carcinoma-- Prognosis
Diagnosis of TC on CNB?--
IDC may have focal tubular morphology Dx: Invasive ductal ca with tubular features with a comment

SLIDE 13 5/23/2015 13
Well-differentiated IDC Radial sclerosing lesions Microglandular adenosis
Tubular Carcinoma-- ddx
Radial Sclerosing Lesion
p63
Tubular carcinoma Radial sclerosing lesion
Distinguishing Pathologic Features for TC and RSL Tubular carcinoma RSL
Distribution Infiltrative Lobulocentric Gland size/shape Slightly irregular, angulated Distorted, elongated, flattened Lumen Open Compressed, open Cytology
Mild atypia, cuboidal to columnar Bland, flat to cuboidal
Luminal content Basophilic secretion; ± calc ± calc Stroma Desmoplastic, elastotic, cellular Fibroelastotic, hypocellular Basement memb.
+, complete ME layer Absent Present Background FEA/ADH/DCIS, LN Benign Biomarkers ER diffusely + ER patchy +

SLIDE 14 5/23/2015 14
Well-differentiated IDC? Well-differentiated IDC?
Well-diff IDC Tubular carcinoma
Irregular glands Slightly irregular, angulated glands ± Trabeculae and ribbons Open glands Branching and anastomosis No branching or anastomosis (may have cribriform glands) Mild to moderate pleomorphism Minimal pleomorphism Stratified cells, loss of polarity Single layer of cells, basal nuclei Sclerotic to desmoplastic stroma Desmoplastic/elastotic stroma
Randomly distributed Hypocellular dense collagenous stroma or fat Uniform small round glands, eosinophilic secretion Cytology
- Single layer, flat to cuboidal cells, clear to amphophilic
cytoplasm, bland round nuclei
Immunophenotype
- MEC markers (p63, SMM, calponin, SMA) –; S100 diffusely +
- ER -
- Laminin and type IV collagen +
Microglandular Adenosis (MGA)

SLIDE 15 5/23/2015 15
Microglandular Adenosis--
Haphazard distribution
Microglandular Adenosis--
Hypocellular collagenous stroma
PAS stain
Microglandular Adenosis--
Uniform small glands, open lumen, eosinophilic secretion
Microglandular Adenosis
SMM calponin Laminin p63

SLIDE 16 5/23/2015 16 Microglandular Adenosis
S100 ER
Distinguishing Pathologic Features for MGA and TC MGA Tubular carcinoma
Distribution Random Infiltrative Gland size/shape Uniform, small, round Slightly irregular, angulated Lumen Open Open Cytology
Bland, flat to cuboidal Mild atypia, cuboidal to columnar
Luminal content Eosinophilic secretion Basophilic secretion; ± calc Stroma Collagenous to fatty Desmoplastic, elastotic, cellular Basement memb. +, complete
ME layer Absent Absent Background Benign FEA/ADH/DCIS, LN Biomarkers ER -, S100 + ER diffusely + (Courtesy of Dr. Timothy Jacobs)
CNB for a Palpable Mass
Microglandular Adenosis
Follow-up Lumpectomy
Regular MGA Atypical MGA Metaplastic ca

SLIDE 17 5/23/2015 17
Regular MGA Atypical MGA Atypical MGA Metaplastic Carcinoma
Metaplastic CA Arising in MGA and Atypical MGA--
Atypical MGA Metaplastic CA MGA S100 Stain Presentation: mass, mammographic calcifications or an incidental microscopic finding Spectrum of MGA, atypical MGA, invasive carcinoma
- Share immunophenotype and genetic alterations
Non-obligate precursor for triple negative carcinoma
- IDC, metaplastic ca (chondroid diff), adenoid cystic ca
Management
- CNB: excision
- Excision: negative margin, careful clinical follow-up
Microglandular Adenosis
(Wen YH et al: Histol Histopathol 2013; Shin SJ et al: AJSP 2009; Khlifeh IM et al. AJSP 2008)

SLIDE 18 5/23/2015 18
Low-grade Adenosquamous Carcinoma (LGASC)
Infiltrative (may resemble RS in some cases) Spindle cellular stroma, prominent lymphoid reaction Glands (long, irregular) and solid squamous nests (comma shaped extension), ± squamous cysts Cytology: bland
- Glands: some with epithelial and myoepithelial cells; variable
squamous diff.
- Solid nests: squamous cells
Low-grade Adenosquamous CA (LGASC)
LGASC-- Infiltrative Growth?
LGASC– Cellular Stroma and Prominent Lymphoid Reaction

SLIDE 19
5/23/2015 19
LGASC-- Glands and Squamous Nests? LGASC-- Squmous Cysts?

SLIDE 20 5/23/2015 20
LGASC-- Squamous Cyst/Nests with Comma-like Extension? LGASC-- Infiltrating Between and Into Lobules MEC markers (p63, SMM, calponin, SMA): consistently variable pattern
- Continuous, discontinuous or absent staining around
glands/epithelial nests in the same lesion
- No tumor shows complete absence of staining by any of the
MEC markers
Squamous cells: p63 and CK5/6 + ER/PR/HER2 negative
LGASC-- Immunophenotype
(Kawaguchi and Shin: AJSP 2012; Boecher W et al: Histopathology 2014)
LGASC– Immunophenotype ?
p63 Calponin SMM

SLIDE 21
5/23/2015 21
p63 SMM
LGASC-- Immunophenotype?
CNB for a Palpable Mass?
Squamous Nests into Lobules Solid Tubules and Nests Cellular Stroma
Prominent Perineural Invasion, Squamous Atypia

SLIDE 22 5/23/2015 22
Triple Stain: p63 +, calponin -, LMWK -
Low-grade adenosquamous carcinoma mimicking a sclerosing lesion Benign fibrosclerosing lesions (SA, radial scar)
- CNB: “low-grade or atypical sclerosing lesion” descriptive dx for
unusual morphologic features or IHC pattern for MEC markers
Syringomatous tumor of the nipple (SyT)
- Similar morphology and immunophenotype
- Location: SyT in superficial skin of nipple/areola; LGASC in
peripheral breast parenchyma
Reactive squamous metaplasia Tubular carcinoma
LGASC-- ddx
An uncommon variant of metaplastic ca May arise de novo or in association with benign sclerosing lesions (RS, sclerosing papilloma) Triple negative Indolent behavior with excellent prognosis
- Local aggressive growth, extremely low metastatic potential
- Rare cases: transition to higher grade ca (spindle cell ca)
- Complete surgical excision; chemotherapy likely not indicated
Low-grade Adenosquamous Carcinoma
Tubular Pattern of ACC: Mimic Benign Glands or IDC

SLIDE 23 5/23/2015 23
Adenoid Cystic Carcinoma (ACC)
Cribriform Pattern Tubular Pattern
Tubular ACC-- Biphasic Epi-Myoepithelial Diff. ACC– Aberrant MEC Expression and Negative ER
p63 ER Calponin
Diffuse pattern Dual cell types-- Myoepithelial-like/basaloid cells Epithelial cells Immunophenotype MEC markers: p63/SMA + & SMM/calponin - in basaloid cells LMW CK (CK7) + in epithelial cells ER/PR/HER2 -
Adenoid Cystic Carcinoma
(Rabban Mod Pathol 2006;19:1351; Foschini Semin Diagn Pathol 2010;27:77)

SLIDE 24 5/23/2015 24
Problem with IHC stains Special types of breast tumors Microglandular adenosis Low-grade adenosquamous carcinoma Adenoid cystic carcinoma Metastatic carcinoma
When a Low-grade “Infiltrative” Epithelial Lesion is ER Negative--
Morphologic alterations secondary to procedures
- Prior needling (CNB, FNA)
- Current procedure (injection for SLN, tissue processing)
Various changes
- Mimic stromal invasion
- Mimic LVI
- Mimic LN metastasis
Factors
- Time interval
- Lesion type: papillary lesion
MEC markers often not helpful
Iatrogenic Small Glandular Lesions
(Phelan S et al: J Clin Pathol 2007)
Mechanical Displacement of DCIS Cells--
Bx tracts
Mechanical Displacement of DCIS Cells-- Tumor cells associated with biopsy site changes

SLIDE 25
5/23/2015 25
Mechanical Displacement of DCIS Cells-- Tumor cells associated with biopsy site changes Epithelial Displacement s/p FNA-- Epithelial cells in stoma and vascular space Epithelial Displacement s/p CNB
Re-excision for Extensive HG DCIS with + Margin

SLIDE 26 5/23/2015 26
SMM
Squamous Metaplasia at Biopsy Site Squamous Metaplasia at Biopsy Site
SMM p63
Squamous Metaplasia at Biopsy Site Squamous Metaplasia at Biopsy Site
Prior DCIS Current Epithelial Lesion

SLIDE 27 5/23/2015 27
CK5/6
Re-excision for DCIS Squamous Metaplasia at the Biopsy Site Lobulocentric
Diffuse and haphazard Sclerosing adenosis Nodular adenosis Radial sclerosing lesion Squamous metaplasia Epithelial displacement Tubular ca & well-diff IDC Microglandular adenosis Low grade adenosquamous ca Adenoid cystic ca
Approach to Small Glandular Lesions of the Breast
Benign sclerosing lesions may exhibit reduced or absent expression in one 1 or more MEC markers MGA lacks expression of multiple MEC markers Some invasive carcinomas (LGASC, ACC) express 1 or more MEC markers
Myoepithelial cell (MEC) markers
It cannot necessarily be concluded that lack of one MEC marker indicates invasion or that expression of
- ne MEC marker supports a benign lesion.
A panel of MEC markers should be used. Lobulocentric
Diffuse and haphazard Sclerosing adenosis Nodular adenosis Radial sclerosing lesion Squamous metaplasia Epithelial displacement Tubular ca & well-diff IDC Microglandular adenosis Low grade adenosquamous ca Adenoid cystic ca ME markers + + + + & -
+ & -
Approach to Small Glandular Lesions of the Breast

SLIDE 28 5/23/2015 28
Lobulocentric
Diffuse and haphazard Sclerosing adenosis Nodular adenosis Radial sclerosing lesion Squamous metaplasia Epithelial displacement Tubular ca & well-diff IDC Microglandular adenosis Low grade adenosquamous ca Adenoid cystic ca ER + + +
+++
- Approach to Small Glandular Lesions of the Breast
Thank you!