Page 1
NEXT-GENERATION IMMUNOHISTOCHEMISTRY FOR SOFT TISSUE TUMORS: FROM DIFFERENTIATION TO MOLECULAR GENETICS
Jason L Hornick, MD, PhD
Director of Surgical Pathology and Immunohistochemistry Brigham and Women’s Hospital Professor of Pathology Harvard Medical School Boston, MA, USA
Disclosures
- Dr. Jason Hornick discloses the following
financial interests:
Consultant to Eli-Lilly and Epizyme
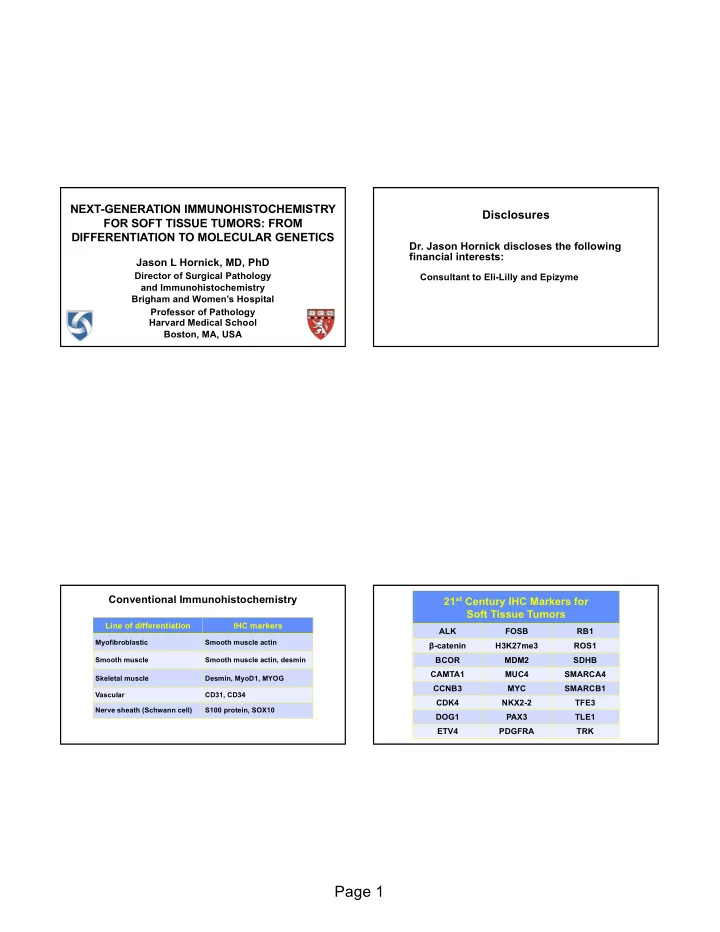
Line of differentiation IHC markers
Myofibroblastic Smooth muscle actin Smooth muscle Smooth muscle actin, desmin Skeletal muscle Desmin, MyoD1, MYOG Vascular CD31, CD34 Nerve sheath (Schwann cell) S100 protein, SOX10