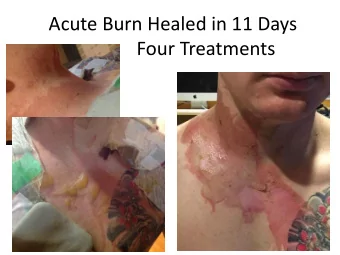
New Treatments in Dermatology Toby Maurer, MD University of - PowerPoint PPT Presentation
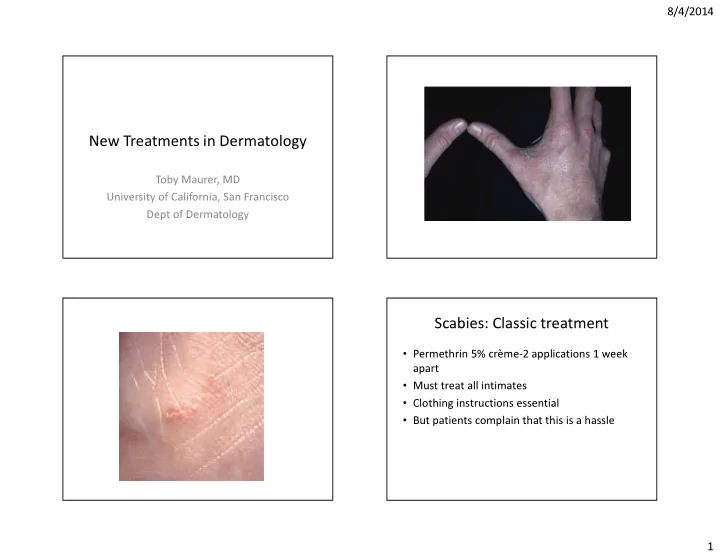
8/4/2014 New Treatments in Dermatology Toby Maurer, MD University of California, San Francisco Dept of Dermatology Scabies: Classic treatment Permethrin 5% crme-2 applications 1 week apart Must treat all intimates Clothing
8/4/2014 New Treatments in Dermatology Toby Maurer, MD University of California, San Francisco Dept of Dermatology Scabies: Classic treatment • Permethrin 5% crème-2 applications 1 week apart • Must treat all intimates • Clothing instructions essential • But patients complain that this is a hassle 1
8/4/2014 Crusted scabies • Scabies mite burden very high • Have treated with malathion ( a pesticide) and ivermectin (an oral medication) • Easier to use and higher success rate-how about using these agents in regular scabies Scabies • Oral ivermectin superior to malathion in adults BUT this is second line drug • While it is easier to give-it is expensive and overuse might lead to resistance • We have seen resistance with Kwell (Lindaine) • First line is still permethrin (elimite) Martin Annals of DermatolVenerology 2010 Dec 2
8/4/2014 New England Journal of Hepatitis C Scabies Treatment • Big global burden-leads to infection and one • Telapravir • Daclatasvir plus of the major reasons for glomerulonephritis • Vaccine? • Sofosbuvir with or without Ribavirin • Stimulates specific protective antibodies as • Able to achieve cure rates up to 98% with opposed to increasing general immunity these drugs NEJM May 2014 • XIAOSONG L. ,WALTON S., MOUNSEY K. Vaccine May 2014 • Telapravir-erythema multiforme, eczema • Sofosbuvir with or without Ribavirin-dry skin 3
8/4/2014 Drug Reaction with Eosinophilia and Systemic Symptoms (DRESS) DRESS Post DRESS • Drug hypersensitivity-monitor LFTs , Cr, Eos • Check TSH 3 months post DRESS • Be aware of cardiac abnormalities • If elevated, start prednisone 60 qd x 10 days then slow taper over as much time as it takes (eosinophil count may help guide taper) 4
8/4/2014 Drug Reactions • Thiazides known to give photodrug reaction • Calcium Channel blockers-associated with non- specific eczematous reactions/itch in the elderly- starts on arms and legs-if you can, switch pt’s to other drugs Summers et al JAMA Dermatol May 2013 • Allopurinol- rare drug reactions but 25% mortality rate-don’t use for hyperuricemia-risk is too high Kim et al Arthritis Care Res April 2013 Guttate Psoriasis Psoriasis • Mounting evidence that cardiovascular disease and psoriasis are associated • Now concern re: kidney disease-increased risk independent of traditional risk factors Risk of moderate to advanced kidney disease in patients with psoriasis: population based cohort study. Wan J1, Wang S, Haynes K, Denburg MR, Shin DB, Gelfand JM. BMJ Oct 2013 5
8/4/2014 Let’s go back in time • The old moist wraps: Used about 25 years ago Corticosteroid and ointment goes directly onto skin Moisten first layer-kerlex, gauze, socks that are cut open-ring out for excess water Dry layer on top-sleep in this overnight Can be done nightly for up to 2 weeks until gone OR Every 5 days-watch for maceration of skin 6
8/4/2014 Food Nursing Education • Not enough evidence to suggest that any • Two nice studies: Great Britain and foods or categories of food contribute to Netherlands atopic dermatitis 9adults) Atopic families who had the benefit of intense • Not enough evidence to suggest that breast nursing education did much better re: quality of feeding reduces risk for developing atopic life and severity indices compared to families dermatitis who just saw the doctor. • Not enough evidence to suggest that holding des Bes et al Acta DermatolVenereol 2011 Jan back on solids or milk after 4-6 months of age reduces risk for developing atopic dermatitis Eczema Guidelines AAD March 2014 • Emollients, emollients • When fail-use topical steroids and maintain only on problem areas • Additives to bath-no benefit except with bleach • Wraps are good in flares • Avoid systemic steroids 7
8/4/2014 • Clobetasol oint qd x 1 wk when severe then • If needed, cyclosporine, methotrexate, • Fluocininide (lidex) x 2 wks then azathioprine and mycophanelate mofetil and ultraviolet light-all useful! • TAC 0.1% oint bid (maintenance) • Antihistamines help with sleep but do not • Aclovate oint or HC !% oint bid face help with itch • No evidence to support or refute its use • Watch in the elderly Cellulitis • Goal in study was to have dermatologists diagnose cellulitis vs other diseases • 635 pts seen-67% had cellulitis N=425 • 33% had other-eczema, lymphedema, lipodermatosclerosis • Of the 425 with cellulitis, 30% had predisposing dermatologic disease • Hospitalization was averted for 96% of those with cellulitis (p.o antiotics) Levell et al Br J of Dermatol (BJD) 2011 Feb 8
8/4/2014 Red legs Take Home Points: • Does the patient really have cellulitis? • Is there an underlying dermatologic cause that contributes to condition-if treated could prevent repeated episodes? • Does this patient require hospitalization? 9
8/4/2014 Recurrent Cellulitis • In study of 274 pts who had at least 2 episodes of cellulits in 3 yrs: • Prophylactic penicillin 250 bid decreased rates of recurrence in treatment gp vs placebo group ( tx=22% vs 37% in placebo gp) • BUT off meds and followed-recurrence rate was the same in both groups. • NEJM Thomas etal. May 2013 Hidraadenitis supparativa • Hidradentitis-go back to strong antiinflammatories like rifampin and clindamycin-12 week course • Moxifloxicin, metranidazole, rifampin-Lambert et al. Dermatology 2011 • Acitretin may have some activity-drug is classically used for psoriasis (original use for TNF blockers Boer et al Br J Dermatol 2011 Jan 10
8/4/2014 Chronic wounds • If not healing and developing thickened or ulcerated skin-biopsy for cancer 11
8/4/2014 • Can it be used in pts with previous zoster-yes • How about use in younger age groups? • Needs to be give within ½ hour of reconstitution • $150.00 for injection • Cost-effectiveness of vaccination against herpes zoster and postherpetic neuralgia: a critical review-Kawai K et al, Vaccine March 2014 • Sunscreens- Australian study randomized -uptake in most communities is only around 30% residents to daily use vs discretionary us -recommended now before giving patients between 1992 and 1996 immunosuppressive drugs like MTX or TNF • Risk for developing any melanoma reduced by blockers JAMA 2011 50% and invasive melanoma risk reduced by 73% • Same trial also showed reduction of risk of developing squamous cell cancer Green et al. J Clin Oncol 2011 Jan 20; 29:257 12
8/4/2014 Tanning Beds • International Agency for Research on Cancer • Comprehensive metaanlaysis found that risk of melanoma (skin and eye) increases by 75% when tanning begins before age 30. • Cite this to your young patients El Ghissassi et al. Lancet Oncol 2009 Aug 10:751 13
8/4/2014 Photodynamic therapy • Place photosensitizer on skin and then use light therapy-increases absorbency of light • Evidence that it changes histologic features of photodamage and changes expression of oncogenes Uses in: • Actinic keratoses • Basal cell cancers • Superiority studies being evaluated • Bagazgoitia et al BJD 2011 July 14
8/4/2014 BCC • New drugs for multiple BCC’s-vismodegib-? SCC development-JAMA Derm May 2014 For superficial BCC’s: • PDT vs imiquimod?- imiquimod better • Imiquimod vs surgery?- surgery better The Telederm Experiment • California Health Care Foundation-can we make it happen in San Francisco area • Primary care provider has any derm question or wants to refer to derm • ALL referrals go through telederm-even if it is a pt followed by derm in past 15
8/4/2014 • Obtains verbal consent from pt • Provider or assistant takes picture and uploads picture • Question can be typed in on web based template at the time of pt visit or later that day, etc • Derm group answers question and primary will get notification that derm report is ready • Provider will get first pass advice-what is it, how to treat, when he/she should see pt back or when to refer OR • Provider will be alerted that pt needs derm appointment and pt will be LINKED into CARE within an appropriate time to be seen in LIVE CLINIC (manned by our dermatologists). • Derm report is part of the electronic medical record 16
8/4/2014 Results to date • Dermatologists from UCSF read the triage • We have completed around 4000 consults • 75% of consults have been successfully consults and they also staff the live clinics at the primary care providers site treated by primary provider with derm guidance-the GPS system • 25% seen in live derm clinic • Wait time at San Mateo was 9 months to see DERM. Now we get consults back in 2 days and live clinics booked within 1 month • Primary providers have learned from one on one consults • Primary providers have had to DO some dermatology • Live dermatology clinic –difficult cases but time has been properly apportioned to see them 17
8/4/2014 • Suspect Hypertrophic lichen planus • Start pt on clobetasol oint bid • Order CBC, LFT’s and G6PD • Look in mouth and genitals-if lesions-set up with GI for endoscopy • Our scheduler will call pt to come in next 3 wks PCP’s reply • Labs obtained, linkage of care to specialists within 1 month ( bonus for hospital), meds started, I learned what this is, what labs to get and that in some circumstances assoc with cancer-can I get CME? 18
Recommend
More recommend
Explore More Topics
Stay informed with curated content and fresh updates.