6/8/2017 1
Masking and Breast Density Can we Quantify Masking Risk?
Nico Karssemeijer Diagnostic Image Analysis Group Radboud University Nijmegen The Netherlands
Disclosures
Volpare Health Solutions (Wellington, New Zealand) co-founder and shareholder Qview Medical (Los Altos, CA) consultant, co-founder and shareholder ScreenPoint Medical (Nijmegen, Netherlands) CEO, co-founder, Shareholder
- What is masking?
- Masking and interval cancers
- Determining the risk of masking in mammograms
- BI-RADS
- Density measurement
- Model based methods
- Breast compression and masking
Overview
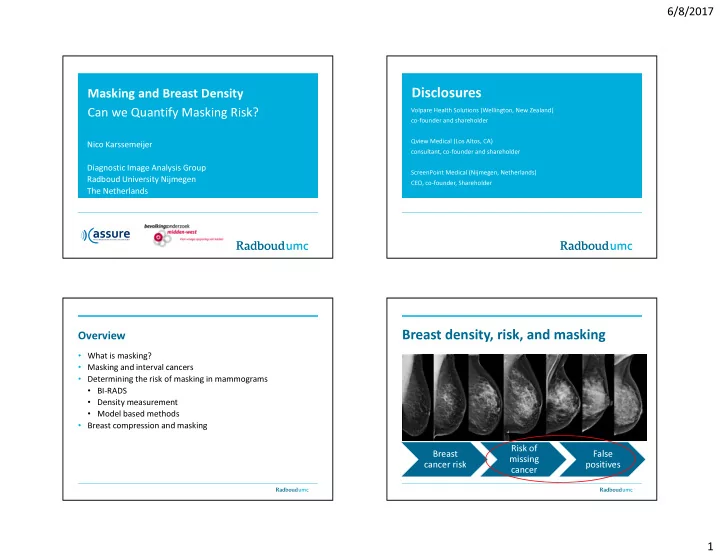
Breast density, risk, and masking
Breast cancer risk Risk of missing cancer False positives