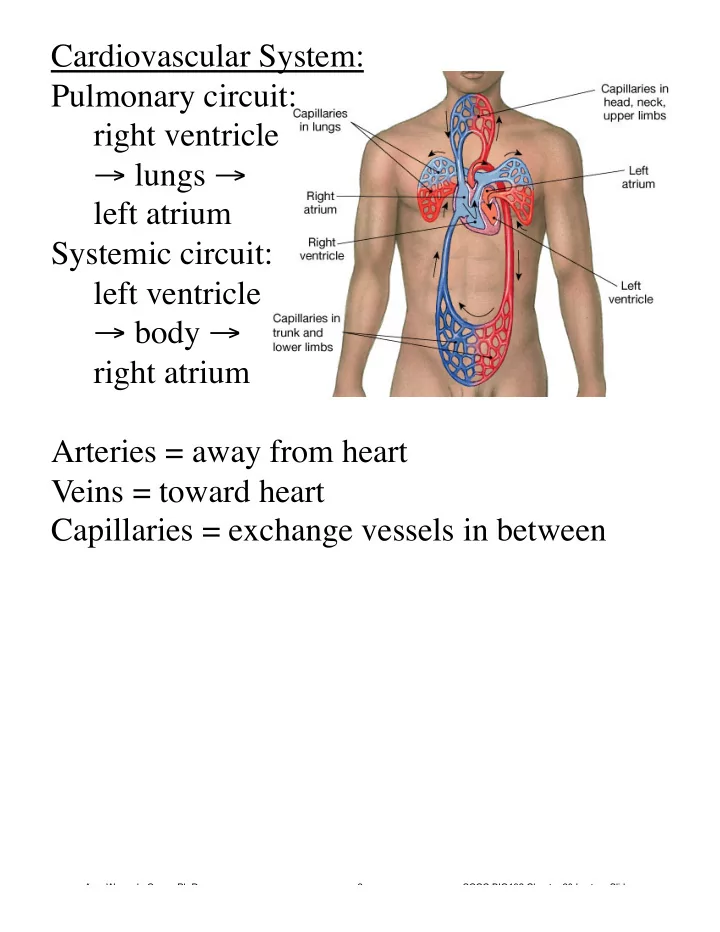
Cardiovascular System: Pulmonary circuit: right ventricle → lungs → left atrium Systemic circuit: left ventricle → body → right atrium Arteries = away from heart Veins = toward heart Capillaries = exchange vessels in between
Amy Warenda Czura, Ph.D. 2 SCCC BIO132 Chapter 20 Lecture Slides