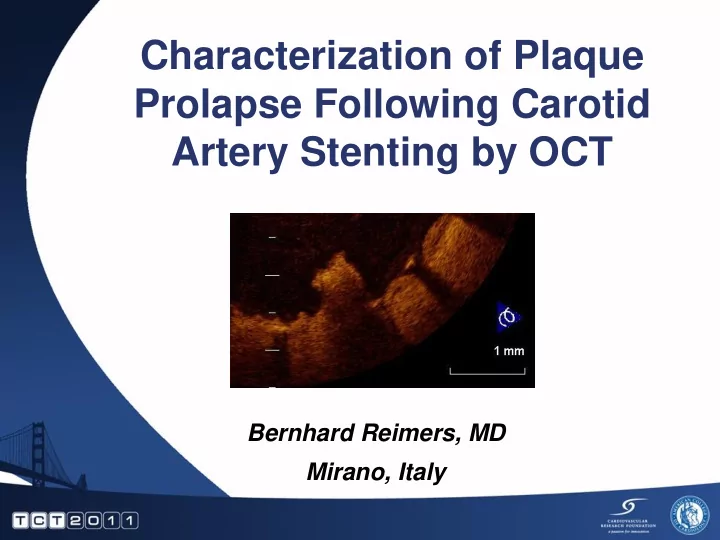
SLIDE 1 Characterization of Plaque Prolapse Following Carotid Artery Stenting by OCT
Bernhard Reimers, MD Mirano, Italy

SLIDE 2
Disclosure Statement of Financial Interest I, Bernhard Reimers DO NOT have a financial interest/arrangement or affiliation with one or more organizations that could be perceived as a real or apparent conflict of interest in the context of the subject of this presentation.

SLIDE 3
Definition
Plaque prolapse is defined as tissue extrusion through the stent struts post- procedure. Brack MJ, et al. Int J Cardiol. 1994;44(1):93- 95

SLIDE 4
Heart: From enzyme rise to heart attack Brain: From ischemic lesions to stroke Possible distal embolization
Consequences of plaque prolapse

SLIDE 5 Relation between plaque components and plaque prolapse after DES implantation: virtual histology –intravascular ultrasound Hong YJ et al. Circ J 2010;74:1142
Necrotic core and fibrotic components were associated with development of PP; and both components in prolapsed plaque were associated with cardiac enzyme elevation after DES implantation.
BMJ Case Reports 2009; Tsui, Lau

SLIDE 6 SPACE
CEA & CAS have additional complications within 30 days
Lancet 2006

SLIDE 7 DW MRI before and 5 days after CAS DESERVE Study

SLIDE 8 Cause of plaque prolapse
Cheese grater effect of stents:
- during deployment,
- during postdilatation (most TCD hits),
- during 30-days post procedure

SLIDE 9 Cheese grating is not always good
Increased plaque prolapse from coronary experience:
- thrombotic lesion
- lipid core
- thin cap over necrotic core
Hung et al; Circ 2010 Differences between soft and hard cheeses plaques

SLIDE 10 Detection of plaque prolapse
Angiography IVUS OCT AHA Journals; BMJ; J Intevent Cardiol In coronary arteries

SLIDE 11 Precise NexStent Xact Acculink Ø = 0.107 mm Ø = 0.118 mm
Ø = 0.128 mm Ø = 0.173 mm
Closed-cell stents Open-cell stents
The concept of plaque scaffolding of stents

SLIDE 12 Emboli Protection Strategies and OCT acquisition
Non Occlusive Technique

SLIDE 13 Emboli Protection Strategies and OCT acquisition
Occlusive Technique

SLIDE 14
1 Positioning of OCT catheter distal to stent

SLIDE 15
2 Careful hand injection of 20cc dye (Ultravist 320) 3 When images ok: pull-back of OCT system

SLIDE 16
4 Hand re-aspiration of dye

SLIDE 17

SLIDE 18 Carotid OCT
After stent in stent with Acculink 6-8 x 40 mm and postdilatation with 5.5 x 20 a 12 atm balloon
Post stent OCT

SLIDE 19
Small ulcers (no clinical determinant of complictions)
Carotid OCT

SLIDE 20 Open cell struts Closed cell struts
Carotid OCT
Open cell stent Closed cell stent

SLIDE 21
Plaque rupture
Carotid OCT

SLIDE 22 Flow artefact
Carotid OCT

SLIDE 23 Carotid OCT
Plaque prolapse: Possible determinants of late complications

SLIDE 24
Carotid OCT before CAS

SLIDE 25
Lesion after stenting

SLIDE 26
Final result after post-dilatation

SLIDE 27 Conclusions (1)
OCT after carotid stenting appears feasible and safe. Using the occlusive technique, better quality images were
- btained with the advantage not to increase the contrast load
Carotid OCT allows collection of important information regarding the stent and plaque behaviour not seen with standard angiography Compared to IVUS less penetration (for plaque characterization), better surface images (for stent evaluation)
Reimers et al.; EuroIntervention 2011
Conclusions

SLIDE 28

SLIDE 29

SLIDE 30

SLIDE 31

SLIDE 32

SLIDE 33
- Interv. Cardiol 2010;2:535
Prolapse Malapposition Prolapse Prolapse Dissection Coronary OCT