9/29/16 1
Ablation of Ventricular Tachycardia: Indications for Use of Endocardial and Epicardial Approaches
Edward P Gerstenfeld MD Professor of Medicine University of California, San Francisco
UCSF
Conflicts
Ø Biosense-webster: research grant, honoraria Ø Medtronic: research grant, honoraria Ø St Jude Medical: research grant, honoraria Ø Boston scientific: honoraria Ø Rhythm diagnostic systems: advisory board
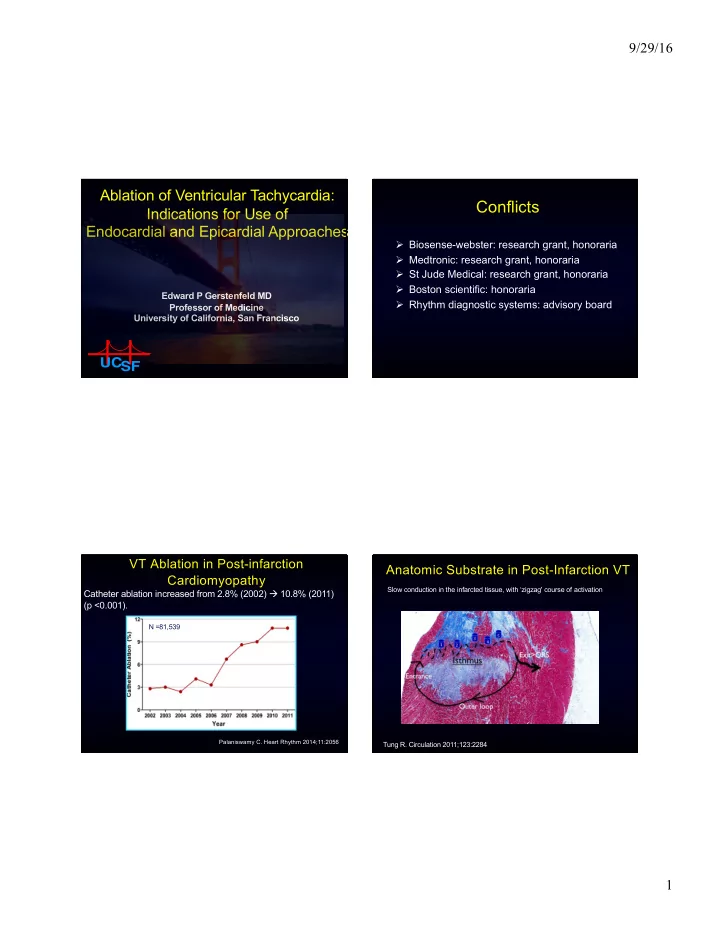
VT Ablation in Post-infarction Cardiomyopathy
N =81,539
Palaniswamy C. Heart Rhythm 2014;11:2056
Catheter ablation increased from 2.8% (2002) à 10.8% (2011) (p <0.001).
deBakker J. Circulation 1988; 77:589
Slow conduction in the infarcted tissue, with ‘zigzag' course of activation Tung R. Circulation 2011;123:2284