SLIDE 1
5/26/2016 1
Vascular Lesions of the Breast
UCSF 32nd Annual Current Issues in Anatomic Pathology and Cytology
Sandra J Shin, MD Professor of Pathology and Laboratory Medicine Chief of Breast Pathology Weill Cornell Medicine
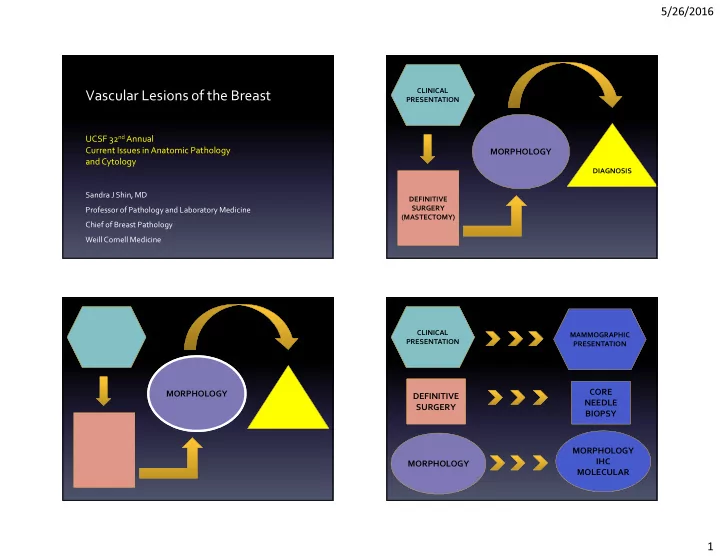
MORPHOLOGY
CLINICAL PRESENTATION DEFINITIVE SURGERY (MASTECTOMY) DIAGNOSIS
MORPHOLOGY
CLINICAL PRESENTATION MAMMOGRAPHIC PRESENTATION