SLIDE 1 10/28/2016 1
Transvaginal Ultrasound Guided Pelvic Procedures
Tara Morgan, MD Assistant Professor of Radiology University of California San Francisco tara.morgan@ucsf.edu
Disclosures
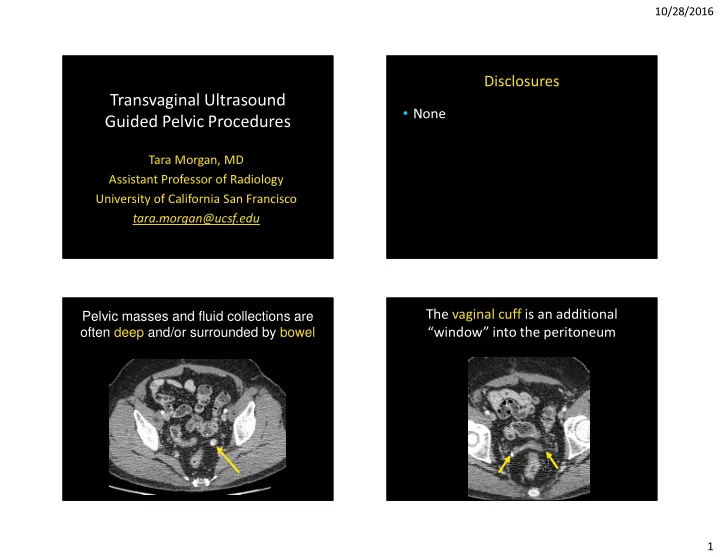
Pelvic masses and fluid collections are
- ften deep and/or surrounded by bowel
The vaginal cuff is an additional “window” into the peritoneum

SLIDE 2 10/28/2016 2
Bladder
Transabdominal vs. Transvaginal Procedures Types
- Biopsy
- Aspiration
- Therapeutic Injection
Patient Selection
- Planning is imperative
- Diagnostic pelvic ultrasound prior to
procedure
- Complication rate is very low
- Usually given conscious sedation
Technique
endocavity needle guide
16-18G needle
location of the needle on the image
programonline.civco.com

SLIDE 3 10/28/2016 3
Biopsies
- Access to the cervix, uterus, vagina,
posterior bladder, adnexa, parametrial/cul-de-sac
- Indeterminate masses
- Suspected cancer recurrence
- Fine needle aspiration vs. core biopsy
Biopsy Case 1
63 year old history mullerian adenosarcoma
Biopsy
Case 1
Biopsy
Case 1
VC

SLIDE 4
10/28/2016 4
Biopsy
Case 1
Biopsy
Case 1
Recurrent Mullerian Adenosarcoma
Biopsy Case 2
36 year old, ovarian cancer
Biopsy
Case 2

SLIDE 5
10/28/2016 5
Biopsy Case 3
56 yo history of serous ovarian cancer
Biopsy
Case 3
High grade carcinoma
T1 T2 fat sat T1 post contrast fat sat
Biopsy Case 4
22 year old female with pelvic pain, referred for mass
Biopsy
Case 4
T2 T1 post contrast fat sat

SLIDE 6
10/28/2016 6
Biopsy
Case 4
Biopsy
Case 4
Case 4
Bladder Paraganglioma
Biopsy Case 5
64 yo pancreatic ca 7 years prior

SLIDE 7 10/28/2016 7
Biopsy Case 5
Metastatic pancreatic cancer
Drainage/Aspiration
- Abscess (gyn vs. non-gyn)
- Hemorrhage
- Ovarian/Peritoneal inclusion cyst
- Serous/Mucinous Neoplasm
- Diagnostic versus symptomatic
- Adjunct or alternative to surgery
Aspiration Case 1
44 yo fever and pelvic pain
Aspiration
Case 1

SLIDE 8
10/28/2016 8
Aspiration Case 1
Post
Aspiration Case 2
24 year old, prior TOA and endometriosis
T2 T1 fat sat post contrast
Aspiration
Case 2
Aspiration
Case 2

SLIDE 9
10/28/2016 9
Aspiration Case 2
Recurrence required drain placement
Aspiration Case 3
55 yo history of vaginal cancer
PET/CT
Aspiration
Case 3
Aspiration
Case 3

SLIDE 10 10/28/2016 10
Aspiration Case 3
Post
R squamous cell, L benign
Therapeutic Injection
- Intra-amniotic injection for ectopic
pregnancy
- Treatment of AVM, fistula
Therapeutic Injection Case 1
C-Section Ectopic
Transvaginal Methotrexate Injection

SLIDE 11
10/28/2016 11
Therapeutic Injection Case 2
23 yo old, s/p D&C and uterine septum removal, AVF ++bleeding
T1 post contrast fat sat
Therapeutic Injection
Case 2
Therapeutic Injection
Case 2
Therapeutic Injection
Case 2

SLIDE 12 10/28/2016 12
Therapeutic Injection
Case 2
Arteriogram of the uterus
Therapeutic Injection
Case 2
T1 post contrast fat sat
Pitfalls
- Poor screening tool
- Prior radiation/scar tissue
- Pelvic ascites
- Technical factors
– Soft masses/collections – Bladder prolapse – Introduction of air BL
Pitfall Case 1
23 year old RLQ pain
T1 post contrast fat sat T2

SLIDE 13
10/28/2016 13
Pitfall
Case 1
Pitfall Case 1 Soft Mass Pitfall Case 2
Pelvic Ascites/Fine Cystic Mass
Pitfall Case 3
40 year old with hx cervical cancer, ?infection vs recurrence

SLIDE 14 10/28/2016 14
Pitfall
Case 3
Pitfall Case 3
2 months later
Pitfall Case 3
Missed Recurrence
Conclusion
- Transvaginal ultrasound is a great
method to access deep pelvic lesions
- Procedures include biopsy, aspiration,
and therapeutic injection
- Some technical limitations can occur

SLIDE 15 10/28/2016 15
1) Transvaginal ultrasound has which advantage over CT?
- A. Better screening/surveillance for
metastatic disease
- B. Larger field of view
- C. Superior resolution of pelvic
structures
- D. Better visualization of bone
- E. Better visualization through gas
filled structures
B e t t e r s c r e e n i n g / s u r v e i l l . . . L a r g e r f i e l d
v i e w S u p e r i
r e s
u t i
p e . . . B e t t e r v i s u a l i z a t i
b
e B e t t e r v i s u a l i z a t i
t h r
. .
0% 0% 3% 0% 97%
Ultrasound
Pyosalpinx
2) What finding may compromise safety of a transvaginal ultrasound guided biopsy?
- A. Prior hysterectomy
- B. Empty bladder
- C. Pelvic Infection
- D. Pelvic Ascites
- E. EPrior radiation
P r i
h y s t e r e c t
y E m p t y b l a d d e r P e l v i c I n f e c t i
P e l v i c A s c i t e s E P r i
r a d i a t i
1% 3% 34% 59% 3%
3) How could this lesion best be sampled for diagnosis?
with ultrasound
guided percutaneous
percutaneous
with CT or ultrasound
be sampled
33 yo with hx of ovarian cancer

SLIDE 16
10/28/2016 16
Percutaneous Approach
Transabdominal US Vaginal Cuff
Transvaginal
Recurrent low serous carcinoma
Tara.morgan@ucsf.edu