In-depth cholera epidemiological study of Cholera in Zimbabwe - - PowerPoint PPT Presentation
In-depth cholera epidemiological study of Cholera in Zimbabwe - - PowerPoint PPT Presentation
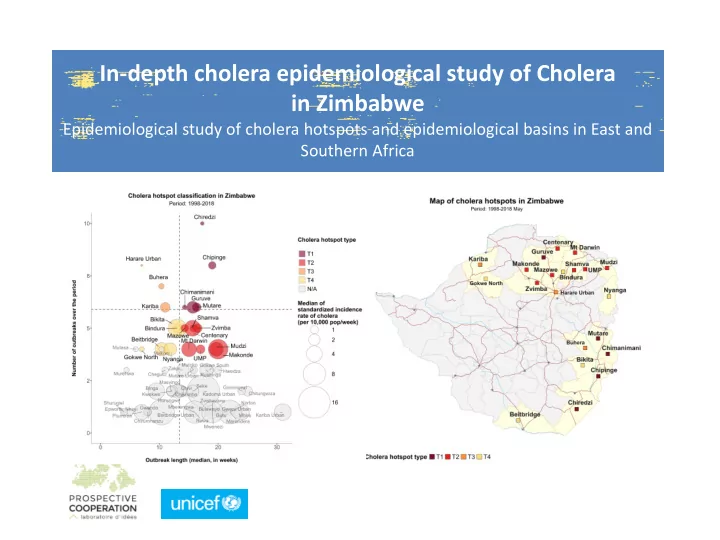
In-depth cholera epidemiological study of Cholera in Zimbabwe Epidemiological study of cholera hotspots and epidemiological basins in East and Southern Africa Prospective Cooperation Cholera Team Cholera specialist Bio-statistic specialist
Prospective Cooperation Cholera Team
2
Cholera specialist Project coordination Bio-statistic specialist Epidemiologist & biologist Field epidemiologist & WaSH engineer Senior epidemiologist Infectious disease specialist & epidemiologist Senior infectious disease specialist & microbiologist
Background
Cholera burden
- Cholera epidemics remain a public health concern in East and Southern Africa
- Approx. 634,000 cases/14,303 deaths (CFR of 2.3%) between 2007-2016
- The brunt of the cholera burden affects a small number of specific zones and
communities: “cholera hotspots” targeted approach (Cf. Ending Cholera Roadmap)
Control and Prevention
- Cholera can be eliminated where access to WASH services are ensured
- Oral cholera vaccine can help provide protection for a population while
sustainable WASH interventions are being implemented
Challenges for sustainable intervention in cholera high-risk areas
- Communities in cholera hotspots are often neglected by WASH development
programs, as WASH sector objectives are coverage (and not health) driven
- Lack of common understanding and knowledge about priority areas
- Lack of donor investment in cholera hotspots
3
UNICEF Strategic Framework in Eastern and Southern Africa
Implementation of the framework hinges on epidemiological studies focused
- n identifying areas regularly affected by cholera outbreaks
4
Development of national and subnational plans 1 Well-targeted capacity development 2 Local-scale social and behaviour change communication 3 Information management for improved monitoring and action 4 Regional coordination and greater cross-border collaboration 5 Knowledge management and operational research 6 Partnerships, public advocacy, social movements and influencers 7
Study region and timeline
5
- Greater Horn of
Africa : Study results by Oct 2018
- Zambesi Basin:
Study results by Oct 2018
Study objectives
- To better understand the local dynamics of cholera at a national and
regional level
– Apply an approach combining field research, epidemiology and genetic analysis of clinical isolates of Vibrio cholerae
- To identify cholera hotspots as well as high-risk populations and
practices for targeted emergency and prevention programs
- To establish effective strategies to combat cholera in Zimbabwe and
neighboring countries
Methods (1/2)
- Cholera case definition (Ministry of Health)
Suspected case:
– In a patient age five years or more, severe dehydration or death from acute watery diarrhea in an area where there is no cholera. – In the context of a cholera epidemic, a suspected case is any person age two years or more with acute watery diarrhea, with or without vomiting.
Confirmed case:
– A suspected case in which Vibrio cholerae serogroups O1 or O139 has been isolated from stool samples.
- Cholera cases and deaths (Ministry of Health, WHO)
– Total number of cases/deaths per district for 1998-2002 and 2004-2006 – Weekly time series of cholera cases and deaths per district for 2003 and 2007- 2018 (missing weekly data for 2015).
- GIS shape files, background layers (UNOCHA)
- Population data from ZIMSTAT 2012 census with a population
growth factor derived from the National Health Profile 2014
- Rainfall data estimated from daily TRMM Multi-Satellite
Precipitation Analysis remote sensing products
7
Methods (2/2)
- Data Analysis Process
– Data cleaning and quality assessment, including missing data and outlier detection – Smoothing and interpolation procedure – Patterns of sporadic cases were removed (e.g., a single case or two to three cases without reported cases during the two weeks before and after). – Two successive outbreaks separated by an inter-epidemic period equal to or greater than six weeks were considered as two separate events. – Outbreak: extraction of the key epidemiological features per outbreak event (onset, peak, duration, incidence, case fatality rate, inter-epidemic period) – Hotspot classification according to recurrence, duration and intensity of cholera
- utbreaks
– Interpretation of the results according to local contexts (literature and national expertise)
8
Dynamics of recent cholera outbreaks
9
Dynamics of recent cholera outbreaks
10
Overview of cholera outbreaks between 1998-2018
- Since 1998, cholera cases have been reported in Zimbabwe almost
every year, with the exception of 2014 and 2017
- Cholera is often reported along the Mozambican and Zambian border
- Major outbreaks in 2008-2009 affected the capital city and almost all
provinces due to a concomitant severe economic crisis, which led to widespread disruption of environmental and health services
- Pattern changed over time with very little cholera notification after
2012 – only sporadic cases reported until a resurgence in 2018
- High AR and CFR registered in rural areas
11
Cholera Seasonality
12
STATE / COUNTY MASHONALAND WEST HARARE MANICALAND MASHONALAND CENTRAL MASVINGO MASHONALAND EAST MIDLANDS MATABELELAND SOUTH MATABELELAND NORTH BULAWAYO Median
- nset
week [min-max] 47 [37-11] 48 [33-13] 50 [28-27] 51 [43-20]
- 51
[32-23]
- 51
[40-20]
- 48
[40-05] 47 [44-05] 47 [41-01] 45 [45-45]
Median outbreak start week Week W45 – W51
(November – mid December)
Risk factors
Lack of adequate access to safe water & sanitation and access to healthcare Unreliable water services (quantity; service interruptions, quality) Contaminated environment (open defecation; Sewer bursts & blockages in urban/periurban areas) Rainy season High population density / population density per borehole Low elevation in high-density neighborhoods Presence / number of markets / bus stations in the neighborhood Individual risk factors: low cholera immunity, weakened immune systems due to HIV and AIDS, and poor nutritional status
High-risk population
Children under five and women of childbearing age Rural populations (AR in rural areas > in urban areas in 2008) Mobile working population (age 15-44) in urban areas Refugees / displaced people in camps High-risk practices & aggravating factors Open defecation (44% in rural areas – MICS 2014) Use of unprotected water sources Body transportation & preparation during burials, consumption of food at funeral feasts Belonging to a religious sect that discourages seeking medical attention Low cholera awareness Limited access to oral rehydration solutions at community level increase the severity of dehydration – and risk of mortality Inadequate surveillance / access to healthcare (61.4% of all reported deaths took place in the community in 2008-2009)
Hotspot classification
Cholera hotspot Definition A geographically limited area (e.g. city, administrative level 2 or health district catchment area) where environmental, cultural and/or socioeconomic conditions facilitate the transmission of the disease and where cholera persists or re-appears
- regularly. Hotspots play a central role in the spread of the disease to other areas.
Source: Interim Guidance Document on Cholera Surveillance Global Task Force on Cholera Control (GTFCC) Surveillance Working Group June 2017 http://www.who.int/cholera/task_force/GTFCC-Guidance-cholera-surveillance.pdf
Hotspot classification
Type Interpretatio n Frequency (Percentile
- f
distribution) Frequency
- utbreaks
Duration (Percentile
- f
distribution ) Duration (number
- f
weeks) Intensity (Percentile
- f
distribution ) Intensity Median Indicende
- ver
time
T1 Highest Priority
- >90
>6
- ≥40
≥13.5
- T2
High Priority
- >70
and <90 >4 and<6
- ≥40
≥13.5
- T3
Med. Priority
- >90
>6
- <40
<13,5
- ≥40
>0,9 T4 Low Priority
- >70
and <90 >4 and <6
- <40
<13,5
- ≥40
>0,9
Table 1: Frequency and duration
- f
cholera
- utbreak
thresholds per hotspot type
Hotspot classification
To be classified as Hotspot, a district must have Frequency of outbreaks > 4 To be classified as Hotspot T1, Frequency > 6 & Duration > 13.5 weeks To be classified as Hotspot T3, Frequency > 6 & Duration < 13.5 weeks but Intensity >0.9 To be classified as Hotspot T2, Frequency > 4 & Duration > 13.5 weeks To be classified as Hotspot T4, Frequency > 4 & Duration < 13.5 weeks but Intensity >0.9 NB: Other Potential Areas of Interest: Buhera – Harare Urban – Makoni, Gwokwe North, Mutasa
Hotspot classification
Total priority areas (21 Hotspots) represent 67.9% of cases (Incl. Harare, Buhera, Gokwe
North)
5 highest-priority hotspots (T1) = 15.9% 13 high-priority hotspots (T1+T2) = 36.1% of cases
PROVINCE DISTRICT POP Masvingo Chiredzi 292305 Manicaland Chipinge 316771 Manicaland Mutare 277851 Mashonaland Central Guruve 131483 Manicaland Chimanimani 143036 Mashonaland West Zvimba 278801 Mashonaland Central Centenary 130158 Mashonaland Central Shamva 131069 Mashonaland Central Mazowe 247457 Mashonaland West Makonde 162752 Mashonaland East Mudzi 141247 Mashonaland East UMP 119368 Mashonaland Central Mt Darwin 225489 Harare Harare Urban 1574345 Manicaland Buhera 260631 Mashonaland West Kariba 43851 Masvingo Bikita 172097 Mashonaland Central Bindura 132732 Manicaland Nyanga 134195 Matabeleland South Beitbridge 84888 Midlands Gokwe North 254773 CASES PROP 5283 4,5 5655 4,8 4398 3,7 1718 1,5 1646 1,4 2238 1,9 1038 0,9 2348 2 684 0,6 7398 6,3 3692 3,1 771 0,7 5602 4,7 16229 13,8 4242 3,6 1564 1,3 3111 2,6 2544 2,2 1158 1 5527 4,7 3039 2,6 DEATHS 194 150 321 66 117 130 43 65 29 209 275 69 180 502 164 51 205 52 95 159 148 FREQ 10 8 6 6 6 5 5 5 5 4 4 4 4 8 7 6 5 5 4 4 4 DUR 17,3 19,0 16,4 15,7 14,3 16,5 15,9 15,7 14,3 20,0 19,7 17,0 15,1 7,0 10,4 11,0 13,2 13,1 11,9 10,4 7,0 INT 0,19 0,87 1,16 2,28 0,29 1,22 0,77 4,01 0,86 6,15 3,05 1,21 3,51 0,05 0,45 1,44 1,36 5,28 2,53 2,74 0,36 HOTSPOT T.1 T.1 T.1 T.1 T.1 T.2 T.2 T.2 T.2 T.2 T.2 T.2 T.2 T.3 T.3 T.3 T.4 T.4 T.4 T.4 T.4
Hotspot classification
Total population in 89 districts is 13,7 million people Target population in 21 Hotspots is 5,2 million people, and carry 67.9% of cholera cases Target population in 13 High priority Hotspots is 2,5 million people
2,000,000 4,000,000 6,000,000 8,000,000 10,000,000 12,000,000 14,000,000 16,000,000
Total Population Hotspot Population 89 Districts 21 Hotspots 100% 67,9%
Hotspot classification
T1: Highest-priority area with cholera outbreaks of high frequency (>90th percentile) and extended duration (≥40th percentile) T2: High-priority area with cholera outbreaks of moderate frequency (between 60th and 90th percentile) and extended duration T3: Medium-priority area with cholera outbreaks of high frequency and short duration (<40th percentile) T4: Low-priority area with cholera outbreaks of moderate frequency and short duration.
Hotspot classification
T1: Highest-priority area with cholera outbreaks of high frequency (>90th percentile) and extended duration (≥40th percentile) T2: High-priority area with cholera outbreaks of moderate frequency (between 60th and 90th percentile) and extended duration T3: Medium-priority area with cholera outbreaks of high frequency and short duration (<40th percentile) T4: Low-priority area with cholera outbreaks of moderate frequency and short duration.
Summary of Key findings
22
Cholera Burden Cholera reported almost every year since 1998 2008-2009 outbreak represent the largest part of the caseload (84% of all cases) Only sporadic cases have been reported since 2012 5 most affected provinces Mashonaland West, Central, East, Manicaland and Masvingo Cholera Seasonality Cholera outbreaks tend to start between November-December Cholera risk increases with the start of the rainy season and decreases with the start of the dry season Cholera Hotspots 2/3 of the cholera caseload reported by 1/5 of the districts 21 identified hotspots (districts) responsible for 67.9% of all cases Only 13 high priority hotspots (T1+T2) responsible for 36,1% of all cases
Use of Study Results (before / during an outbreak)
23
Justification for a targeted intervention in Cholera hotspots (even if not yet affected) Cholera hotspots are at higher risk (probability) of being affected Once affected, cholera hotspots are more vulnerable to cholera transmission (higher intensity and duration of cholera outbreaks) Cholera hotspots may be responsible for the spread of cholera to other districts Targeting cholera hotspots to increase preparedness/prevention in high-risk areas. Increase cholera awareness & prevention at the community level Early detection & referral of suspected cholera cases – through community-based surveillance Give access to early rehydration through community oral rehydration therapy Increase the readiness of the health system (training of health workers, stocks, identification of location for CTCs, CTUs, ORPs, etc.)
Use of Study Results (medium- to long-term)
The priority strategic actions should include early detection, community- based surveillance, cross-border activities, and preparedness plans and actions in 21 identified cholera hotspots (Type 1 to 4) Mid-to-long term WASH and social mobilization activities (3-10 years) should be implemented in priority districts regularly affected with significant
- utbreak duration: Type 1 and Type 2
The priority hotspots (Type 1 and Type 2) comprise 13 districts with both urban and rural features which account for 36.1% of the disease burden. Those cholera foci host approximately 2,600,000 people (19% of the total estimated population) An identification of transmission foci at a finer geographical scale (e.g., city section, village) within the priority districts is necessary to better target the at-risk population.
24
Limitations
Missing time series (before 2003 and 2004-2006) may give extra weight to 2008-2009 cholera outbreak episode
25
Opportunities
Identify cholera hotspots and engage in a targeted approach (Cf. Ending Cholera Roadmap) Mainstream epidemiological findings into national policies and gain national commitment from the WASH and Health sectors Provide decision makers with evidence-based information to implement efficient prevention and control activities Mobilize resources for long-term (WASH and health) investments in hotspots as part of the cholera prevention program
- Role of Country office and partners, Regional Office, GTFCC
26
27