4/5/2014 1
Soft Tissue Coverage for the Diabetic Foot
Scott L. Hansen, M.D. Chief, Plastic and Reconstructive Surgery San Francisco General Hospital
Diabetic foot wounds/ulcers
- Neuropathy
– Sensory: loss of protective sensation – Motor: alteration in foot mechanics – Autonomic: dry, cracked skin
- Decreased immune response
– Infection
- Peripheral vascular disease
– Local hypoxia – **Can’t reconstruct until adequate perfusion!
Hansen 2014
General Management
- Staged debridement's with Vascular,
Orthopaedic and Podiatric Surgery
- Assess components of defect
- Continue until wound clean
- Amt. of debridement depends on perfusion
- Wound VAC used as bridge
- Amputation vs. Limb salvage vs. preservation
- f length
Hansen 2014
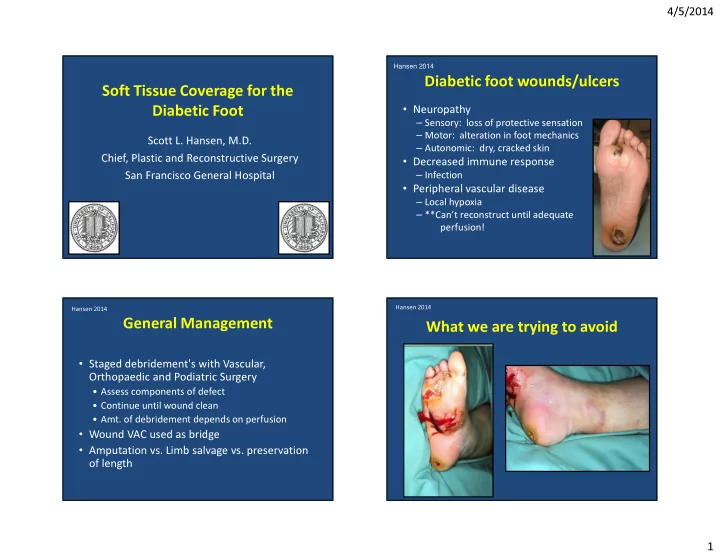
What we are trying to avoid
Hansen 2014