Normal Normal Osteoporosis Osteoporosis
Bone Density Measurement Normal Normal Osteoporosis Osteoporosis - - PowerPoint PPT Presentation
Bone Density Measurement Normal Normal Osteoporosis Osteoporosis - - PowerPoint PPT Presentation
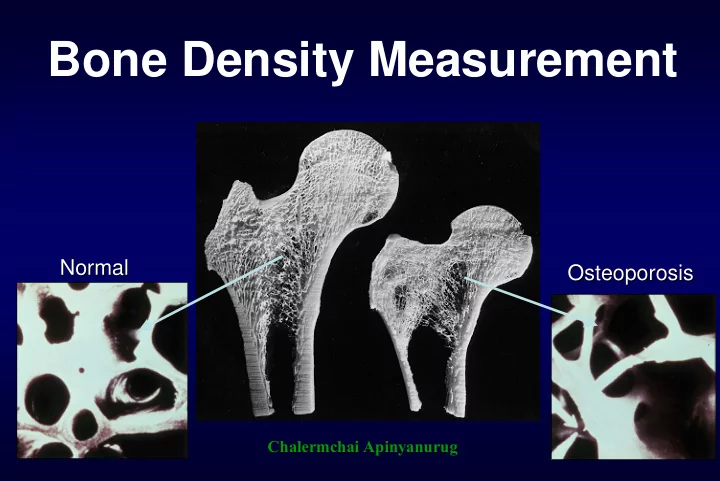
Bone Density Measurement Normal Normal Osteoporosis Osteoporosis Chalermchai Apinyanurug Who should receive BMD testing? National Osteoporosis North American Menopause American Association of Foundation Society Clinical Endocrinolgist
National Osteoporosis Foundation North American Menopause Society American Association of Clinical Endocrinolgist
- All women age ≥ 65 yr
- Younger PM women
with ≥ 1 risk factor
- PM women who
present with fractures
- All women age ≥ 65 yr
- All women with
medical causes of bone loss
- Younger PM women
with ≥ 1 risk factor
- All women age ≥ 65 yr
- All women age ≥ 40 yr
who have sustained a fracture unrelated to major trauma
- All peri- and PM
women who have risk factors for fracture or bone loss
Who should receive BMD testing?
Indications for Bone Mineral Density (BMD) Testing From ISCD 2006
- Women aged 65 and older, Men aged 70 and older
- Postmenopausal women under age 65 with risk factors
- Adults with a fragility fracture
- Adults with a disease or condition associated with low bone
mass or bone loss
- Adults taking medications associated with low bone mass
- r bone loss
- Anyone being considered for pharmacologic therapy
- Anyone being treated, to monitor treatment effect
- Anyone not receiving therapy in whom evidence of bone
loss would lead to treatment
Women discontinuing estrogen should be considered for bone density testing according to the indications listed above
Densitometry Technologies
Central BMD Measurements
– QCT – DEXA
Peripheral BMD Measurements
– Conventional X-ray – RA – radiographic absorptiometry – X-Ray Radiogrammetry – Ultrasonometry – Peripheral DEXA
Routine radiographic
–Low Radiation dose –Insensitive: bone loss is apparent only after a 30% loss
- measures the optical
density
- small, inexpensive
- fingers only
- poor hip fracture prediction
Radiographic Absorptiometry
- Width of cortical bone in fingers
using standard x-ray
- Can be added to existing mammo /
x-ray system (need computer and scanner)
- fingers only
- poor hip fracture prediction
Radiogrammetry
QCT : Quantitative CT
Disadvantage
- High radiation dose
- Less precise than DXA (2-5%)
- Large accuracy errors (15%)
- Expensive
Quantitative Ultrasound of Calcaneus
Advantage
- Portable
- Low costs
- Less time-consuming
- No radiation
- No need well-trained technician
- May predict fracture
Disadvantage
- Not a gold standard
- Diagnostic performance
(High specificity but low sensitivity)
Investigations of osteoporosis : Update 2007
What’s new in DXA equipment's?
New Detector : Direct-Digital Cadmium Zinc Telluride (CZT) Better image quality Low X-ray exposure High accuracy and precision
New technique : One Positioning
One Position, 3 Scans
- AP Spine
- Left Femur
- Right Femur
Old
New DXA equipment : Better Image Quality
New
New DXA equipment : Better Image Quality
Old New
New Asian Reference Database
- China
- Korea
- Indonesia
- Japan
- Thai
New software : Computer Assisted Densitometry
- Automatic verification
– Positioning – Bone edges – Analysis regions – Artifacts
- Clinical Benefits
– Reduce errors – Better scan evaluation
- BMD results
– Previous results – Reference Data Comparison – Trending – Bone strength assessments
- Hip Axis Length
- Femur Strength Index
New Report
New Hip Assessment
- Hip Axis Length
- Upper Neck
- Dual femur study
- Femur Strength Index
“A Better Way to Look at the Femur”
Osteoporosis International. January, 2006
Dual Femur study : Improved Diagnosis and Treatment Decisions
American Society for Bone and Mineral Research : ASBMR 2005
Femur Strength Index
- 2,506 women. > 50 yr.
- significant predictors of hip fracture
- Power for predicting fracture was improved by
combining T-score, FSI, and HAL compared with T- score alone.
Osteoporosis International. January, 2006
Body Composition Methods
Underwater Weighing (Hydrodensitometry) DXA (Dual-energy X-Ray Absorptiometry) BIS Near Infrared Interactance Air Displacement Imaging Methods (CT, MRI) Anthropometry BIA (Bioelectrical Impedance Analysis)
Body Composition with DXA
- Directly measures fat, lean, and bone mass
- Monitoring impact of treatment and exercise/diet
regimens.
- Android/Gynoid Ratio identifies women
with cardiovascular disease
- Better than cholesterol, better than
triglycerides
Body Composition and Cardiovascular Disease
Ragi et al. ASBMR 2005
Estimated Total Body % Fat from Spine and Femur Scans
ASBMR 2005
Osteoporosis
Normal Bone Mass
Low Bone Mass (Osteopenia)
- 4.0 -3.5 -3.0 -2.5
- 2.0 -1.5 -1.0
- 0.5 0 +0.5 +1.0
Assessment of Fracture Risk and Its Application to Screening For Postmenopausal Osteoporosis WHO Study group; 1994.
Interpreting T-scores (WHO)
Correlates With Lifetime Fracture Risk for Caucasian Women
Clinical Risk Score
Index value = 0.2 x (weight - age), then drop the decimal digit
Osteoporosis Self-Assessment Tool for Asians (OSTA) Research Group Osteoporos Int 2001;12:699-705
Osteoporosis Self-Assessment Tool for Asians (OSTA)
OSTA index ≤ -1: High risk > -1: Low risk
- 21 clinics, 8 countries: 860 PM women
- 59% Chinese, 18% Korean, 11% Thai, 8% Filipinos,
4% Indian, Malay and others OSTA index < -4: High risk
- 1 to -4 : Medium risk
> -1: Low risk
Countries N Age Sens Spec PPV Filipinos
1465 40-89 90 66 23
Singapore
135 57-80 97 43 34
Thai
Khon Kaen Songkhla 322 388 45-84 43-91 97 93 (93) 54 61 (30) 21 24 (15)
Original
860 45-88 91 45 21
Chinese
722 1127 1101 43-81 88 54 34
Japanese
47-91 90 38-43 NA
Korean
48-87 87 67 24
Validation of OSTA in Asians
Sens: Sensitivity, Spec: Specificity, PPV: Positive predictive value
Khon Kaen Osteoporosis Study (KKOS) scoring system
Age (y) Score Weight (kg) Score < 45 45 - 49 50 - 54 55 - 59 60 - 64 65 - 69 70 - 74 75 - 79 80 - 84 85 – 89 > 90 + 7.5 + 6.0 + 4.5 + 3.0 + 1.5
- 1.5
- 3.0
- 4.5
- 6.0
- 7.5
< 30 30 - 34 35 - 39 40 - 44 45 - 49 50 - 54 55 - 59 60 - 64 65 - 69 70 - 74 75 - 79 80 - 84 85 - 89 > 90
- 14
- 12
- 10
- 8
- 6
- 4
- 2
+ 2 + 4 + 6 + 8 + 10 + 12
KKOS score
- high risk ≤ -1
- low risk > -1
Sensitivity 86% Specificity 65%
1- Specificity
0.0 0.2 0.4 0.6 0.8 1.0Sensitivity
0.0 0.2 0.4 0.6 0.8 1.0AUC 0.85
Pongchaiyakul C. J Med Assoc Thai 2004;87:910-6.
Probability (%) of having osteoporosis for a given Age and Body weight
Weight (kg) < 45 45-49 50-54 55-59 60-64 65-69 70-74 75-79 80-84 85-89 > 90
< 30 58.7 67.4 75.0 81.3 86.3 90.2 93.0 95.1 96.6 97.6 98.3 30-34 47.5 56.8 65.6 73.5 80.1 85.4 89.5 92.5 94.7 96.3 97.4 35-39 36.6 45.6 54.9 63.8 71.9 78.8 84.4 88.7 91.9 94.3 96.0 40-44 26.9 34.8 43.6 52.9 62.0 70.3 77.5 83.3 87.9 91.3 93.9 45-49 19.0 25.4 33.0 41.7 51.0 60.2 68.7 76.1 82.2 87.0 90.7 50-54 13.0 17.8 23.9 31.3 39.8 49.0 58.3 67.0 74.6 81.0 86.1 55-59 8.7 12.1 16.7 22.5 29.7 38.0 47.1 56.4 65.2 73.1 80.0 60-64 5.7 8.1 11.3 15.6 21.2 28.1 36.2 45.1 54.4 63.4 71.6 65-69 3.7 5.3 7.5 10.5 14.6 19.9 26.5 34.4 43.2 52.5 61.6 70-74 2.4 3.4 4.9 7.0 9.8 13.7 18.7 25.0 32.6 41.3 50.5 75-79 1.5 2.2 3.2 4.6 6.5 9.2 12.8 17.5 23.6 30.9 39.4 80-84 1.0 1.4 2.1 3.0 4.2 6.0 8.5 11.9 16.4 22.2 29.3 85-89 0.6 0.9 1.3 1.9 2.7 3.9 5.6 7.9 11.1 15.4 20.9 > 90 0.4 0.6 0.8 1.2 1.8 2.5 3.6 5.2 7.4 10.4 14.4
Age (yr)
High risk Intermediate risk Low risk
10 20 30 40 50 60
Prevalence of osteoporosis by DXA (%) OSTA Score QUS of calcaneus (T-score)
<-2.5 >-2.5 Low risk (>-1) High risk (<-1)
Figure 1. Prevalence of osteoporosis (by DXA) according to QUS of calcaneus and OSTA score
2.9 14.3 (OR: 5.6) 56.7 (OR: 43.7) 21.4 (OR: 9.1)
10 20 30 40 50 60 70
Prevalence of osteoporosis by DXA (%) KKOS Score QUS of calcaneus (T-score)
<-2.5 >-2.5 Low risk (>-1) High risk (<-1)
Figure 2. Prevalence of osteoporosis (by DXA) according to QUS of calcaneus and KKOS score
2.3 16.7 (OR: 8.6) 58.6 (OR: 60.9) 20.7 (OR: 11.2)
Osteoporosis International 2007;18(4):525-31.
QUS T-score (SD) Weight (kg) Age (yr)
- 4
- 3
- 2
- 1
50 0.49 0.33 0.20 0.12 0.07 55 0.59 0.43 0.28 0.17 0.10 60 0.68 0.53 0.37 0.23 0.14 65 0.77 0.63 0.47 0.32 0.19 70 0.83 0.72 0.57 0.41 0.27 75 0.88 0.79 0.67 0.51 0.35 80 0.92 0.85 0.75 0.61 0.45 85 0.94 0.90 0.82 0.70 0.55 50 0.28 0.17 0.10 0.05 0.03 55 0.37 0.24 0.14 0.08 0.04 60 0.47 0.32 0.20 0.11 0.06 65 0.57 0.41 0.27 0.16 0.09 70 0.67 0.51 0.36 0.22 0.13 75 0.75 0.62 0.45 0.30 0.18 80 0.82 0.71 0.56 0.40 0.25 85 0.87 0.78 0.65 0.50 0.34
50 kg 40 kg
Predicted probability of having osteoporosis for a given age, weight and QUS
QUS T-score (SD) Weight (kg) Age (yr)
- 4
- 3
- 2
- 1
50 0.49 0.33 0.20 0.12 0.07 55 0.59 0.43 0.28 0.17 0.10 60 0.68 0.53 0.37 0.23 0.14 65 0.77 0.63 0.47 0.32 0.19 70 0.83 0.72 0.57 0.41 0.27 75 0.88 0.79 0.67 0.51 0.35 80 0.92 0.85 0.75 0.61 0.45 85 0.94 0.90 0.82 0.70 0.55 50 0.28 0.17 0.10 0.05 0.03 55 0.37 0.24 0.14 0.08 0.04 60 0.47 0.32 0.20 0.11 0.06 65 0.57 0.41 0.27 0.16 0.09 70 0.67 0.51 0.36 0.22 0.13 75 0.75 0.62 0.45 0.30 0.18 80 0.82 0.71 0.56 0.40 0.25 85 0.87 0.78 0.65 0.50 0.34
50 kg 40 kg
Predicted probability of having osteoporosis for a given age, weight and QUS
Points
10 20 30 40 50 60 70 80 90 100
Age
35 45 55 65 75 85
Weight
95 90 85 80 75 70 65 60 55 50 45 40 35 30
QUS
4 3 2 1
- 1
- 2
- 3
- 4
- 5
Total Points
40 80 120 160 200 240 280
Linear Predictor
- 8
- 6
- 4
- 2
1 2 3 4 5
Risk of Osteoporosis
0.01 0.1 0.3 0.6 0.8 0.95 0.99
Female: 70 yr, 50 kg, QUS T-score = -3 SD
48 67 78
~0.5 48+67+78 =193
193
110
Female Age 70 yr BW 50 kg QUS T-sc = -3
Easy Nomogram
Risk of Osteoporosis
Risk of osteoporosis
0.3 0.1 0.05 0.01 0.6 0.8 0.9 0.99
0.5
QUS T-scores Clinical risk scores