9/30/2016 1 A Bridge to Life
MCS: Yesterday, Today and Beyond
Michele Kassemos, RN BSN Mechanical Circulatory Support UCSF Medical Center
MCS at UCSF Medical Center
Mechanical Circulatory Support
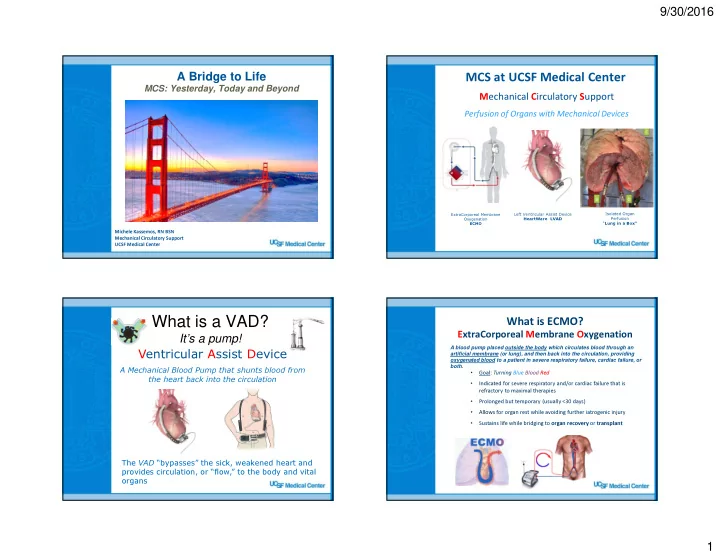
Perfusion of Organs with Mechanical Devices
Left Ventricular Assist Device HeartWare LVAD ExtraCorporeal Membrane Oxygenation ECMO Isolated Organ Perfusion “Lung in a Box”
What is a VAD?
It’s a pump! Ventricular Assist Device
A Mechanical Blood Pump that shunts blood from the heart back into the circulation The VAD “bypasses” the sick, weakened heart and provides circulation, or “flow,” to the body and vital
- rgans
What is ECMO?
ExtraCorporeal Membrane Oxygenation
- Goal: Turning Blue Blood Red
- Indicated for severe respiratory and/or cardiac failure that is
refractory to maximal therapies
- Prolonged but temporary (usually <30 days)
- Allows for organ rest while avoiding further iatrogenic injury
- Sustains life while bridging to organ recovery or transplant
A blood pump placed outside the body which circulates blood through an artificial membrane (or lung), and then back into the circulation, providing
- xygenated blood to a patient in severe respiratory failure, cardiac failure, or
both.