Welcome to the BOOST Collaborative!
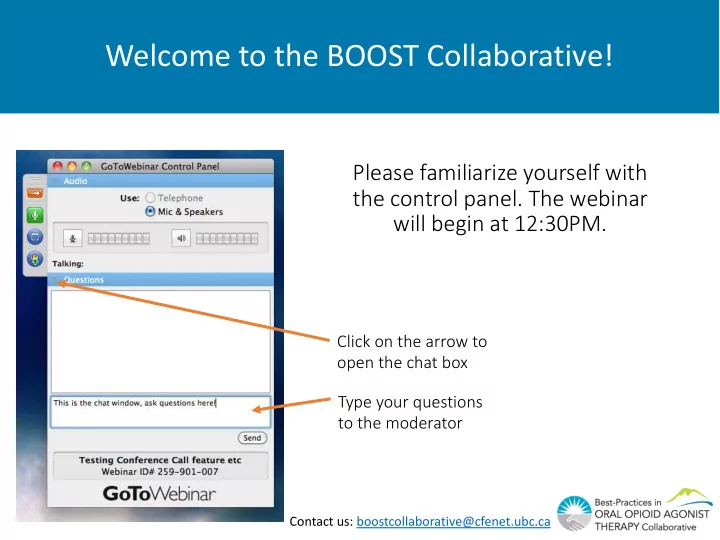
Please familiarize yourself with the control panel. The webinar will begin at 12:30PM.
Contact us: boostcollaborative@cfenet.ubc.ca
Type your questions to the moderator Click on the arrow to
- pen the chat box
Welcome to the BOOST Collaborative! Please familiarize yourself with - - PowerPoint PPT Presentation
Welcome to the BOOST Collaborative! Please familiarize yourself with the control panel. The webinar will begin at 12:30PM. Click on the arrow to open the chat box Type your questions to the moderator Contact us:
Contact us: boostcollaborative@cfenet.ubc.ca
Type your questions to the moderator Click on the arrow to
Friday, Aug 31st 2017 12:30 – 1:30 PM
Type your questions to the moderator Click on the arrow to
You will be muted during the Webinar We will be recording the webinar
Laura Beamish Introductions and overview 5 min
Quality improvement fundamentals 15 min Danielle Cousineau Laura Beamish The BOOST Collaborative Methodology and preparation checklist 15 min Questions and discussion 20 min
effects, stable on low dose, etc.)
55 60 70 85 90 75 100 100 100 10 20 30 40 50 60 70 80 90 100 Baseline Month 1 Month 2 Month 3 Goal Outcome Process
2 4 6 8 10 12 Reason for not being on optimal dosing Adherence Stable on low dose New start Other
Pareto chart Run chart
Change #1 enacted goal line
Da Danielle Cou Cousineau, , RN Qua Quality Impr mproveme ment Cons nsul ultant, BC Centre for Excellenc nce in n HIV/AIDS La Laura Beamish, , MSc Qua Quality Impr mproveme ment Coordi dina nator, BC Centre for Excellenc nce in n HIV/AIDS
provide equitable access to integrated, evidence-base opioid use disorder care to help our collective population achieve:
Aim Primary Drivers Secondary Drivers
By July 1st, 2018 we aim to provide equitable access to integrated, evidence-based care to help our population of clients with opioid use disorder achieve: 95% initiated on oOAT 95% retained in care for ≥3 months 50% average improvement in Quality of Life score Education OAT Treatment Leadership Medical Care Engagement High quality Accessible Relevant Time to access Treatment options Optimal dosing Linkage between programs Treatment duration Accountability Screening Access to leadership Engaged leadership Intake Transitions in care Follow-up Trauma-informed practice Matching acuity of services to need Clinic processes and mandate Patient medical home Cultural competency Social determinants of health
team will base what it is that you want to accomplish (aim) and for whom you will measure key quality indicators.
1. Diagnosis and Treatment Initiation
2. Treatment Retention and Optimal Dosing
3. Quality of Life and Bundle of Care
Type your questions to the moderator Click on the arrow to
Laura Beamish: lbeamish@cfenet.ubc.ca Danielle Cousineau: danielle.cousineau@shaw.ca Cole Stanley: cole.stanley@vch.ca Angie Semple: asemple@cfenet.ubc.ca CONTACT US: boostcollaborative@cfenet.ubc.ca VISIT THE WEBSITE: http://www.stophivaids.ca/oud-collaborative
strategies from population health promotion and the Chronic Care Model. Barr VJ, Robinson S, Marin-Link B, Underhill L, Dotts A, Ravensdale D, Salivaras S. Source: Vancouver Island Health Authority.
http://www.bccsu.ca/wp-content/uploads/2017/06/BC-OUD-Guidelines_June2017.pdf