1
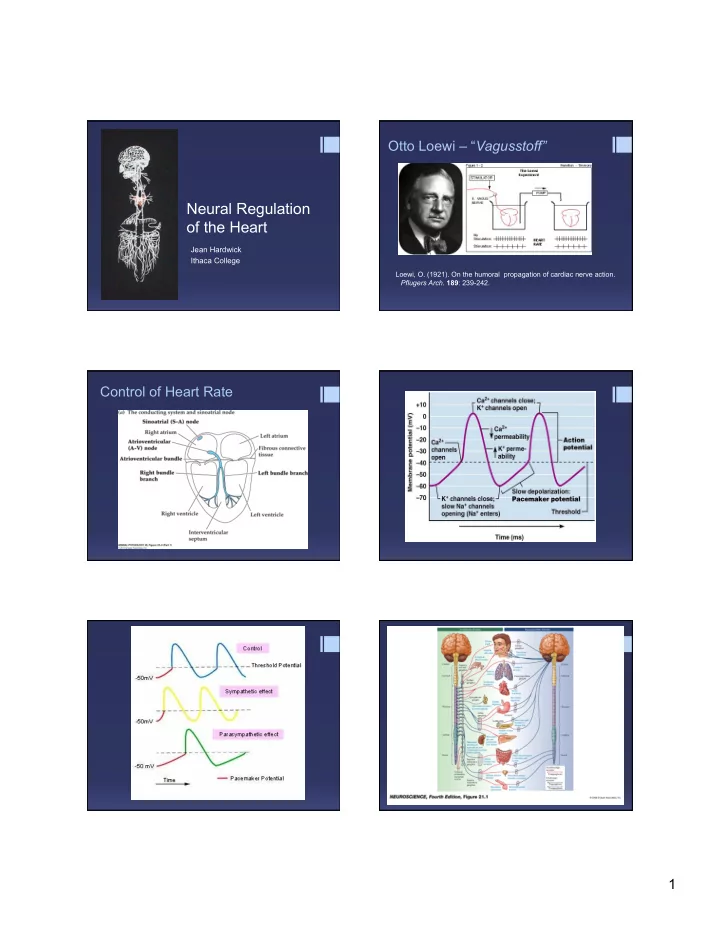
Neural Regulation
- f the Heart
Jean Hardwick Ithaca College
Otto Loewi – “Vagusstoff”
Loewi, O. (1921). On the humoral propagation of cardiac nerve action. Pflugers Arch. 189: 239-242.
of the Heart Jean Hardwick Ithaca College Loewi, O. (1921). On the - - PDF document
Otto Loewi Vagusstoff Neural Regulation of the Heart Jean Hardwick Ithaca College Loewi, O. (1921). On the humoral propagation of cardiac nerve action. Pflugers Arch. 189 : 239-242. Control of Heart Rate 1 Cardiac Ganglion
Jean Hardwick Ithaca College
Loewi, O. (1921). On the humoral propagation of cardiac nerve action. Pflugers Arch. 189: 239-242.
Target Target Preganglionic neuron Postganglionic neuron
CNS Preganglionic Neurons Parasympathetic Postganglionic Neurons Cardiac Target Cells Sympathetic Postganglionic Fibers Cardiac Sensory Neurons
PACAP 1-27 28-38
NOS
Ca++ Guanylate Cyclase
cGMP
Preganglionic Fibers Postganglionic Fibers Sensory Afferents Mast cells Sympathetic Postganglionic Fibers
Mawe, et al (1996) Cell Tissue Res 285:281.
PACAP 27 MAP2
“puffer” containing test substance Preganglionic fiber Postganglionic neuron Phasic Neuron
Tonic Neuron
Stimulus (nA)
0.0 0.2 0.4 0.6
AP Frequency (Hz)
2 4 6 8 10 12 14
Control Histamine, # # # # # #
1 mM Cs+ 1 mM Ba2+ 1 mM 4-AP 5 mM TEA
Control Beth
Control NE
Preganglionic fiber Postganglionic neuron
(N=6)
(N=6)
Horackova, M. et al. (2004) Am J Physiol Heart Circ Physiol 287: H1599-H1608
Control Chronic MI nNOS and MAP2
%nNOS cells 5 10 15 20 25 Control MI Sham surgery PO
# #
IHC - % nNOS Neurons
0 ¡ 0.5 ¡ 1 ¡ 1.5 ¡ 2 ¡ 2.5 ¡ 3 ¡ 3.5 ¡ 4 ¡ 4.5 ¡ 5 ¡ Control ¡ Sham ¡ MI ¡ PO ¡ Rela9ve ¡Change ¡in ¡mRNA ¡Expression ¡
qPCR – nNOS mRNA
Preganglionic fiber Postganglionic neuron
CONTROL MI PO RMP (mV)
EPSP amplitude (mV) 6.8 ± 0.4 6.6 ± 0.6 5.6 ± 0.8 N 17 19 17
No significant differences
FTS 20 Hz
Shannon Ryan ‘12, Kristen Levin ’12, Natasha Petersen ‘12, Rich Kintzing ‘12 Chris Palmer ‘11, Samantha Corrado ‘11, Phil Feinberg ‘11 Melanie Powers Fraites ‘01, Ally Girasole ‘10 Not Pictured: Caitlin Baran ‘09 Lauren Houdek ’09 Stephanie Hinsvark ‘12
The Heart Nebula……..