12/2/2016 1
Give Medications or Laser a Trial First
Yvonne Ou, MD Assistant Professor of Ophthalmology University of California, San Francisco
No financial interests to disclose
Arguments for giving medications or laser a trial first!
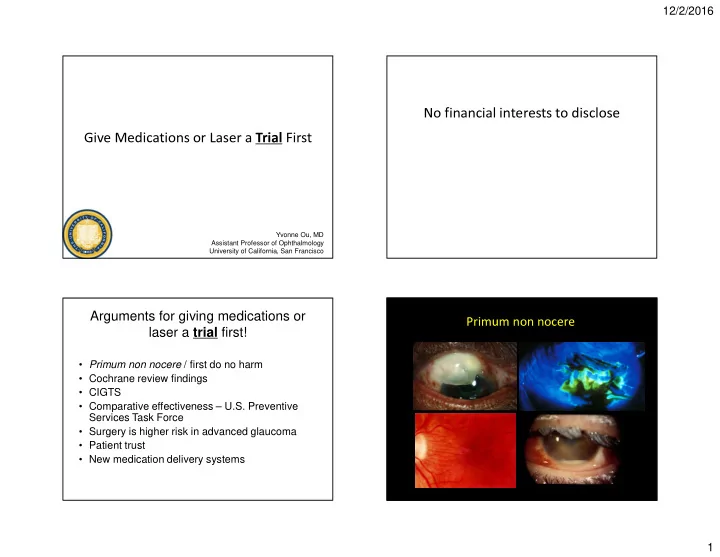
- Primum non nocere / first do no harm
- Cochrane review findings
- CIGTS
- Comparative effectiveness – U.S. Preventive
Services Task Force
- Surgery is higher risk in advanced glaucoma
- Patient trust
- New medication delivery systems