SLIDE 1
Neonatal Isoerythrolysis Pathogenesis
- Immune mediated hemolytic anemia
- Mediated by maternal anti-RBC antibodies
- Colostrum
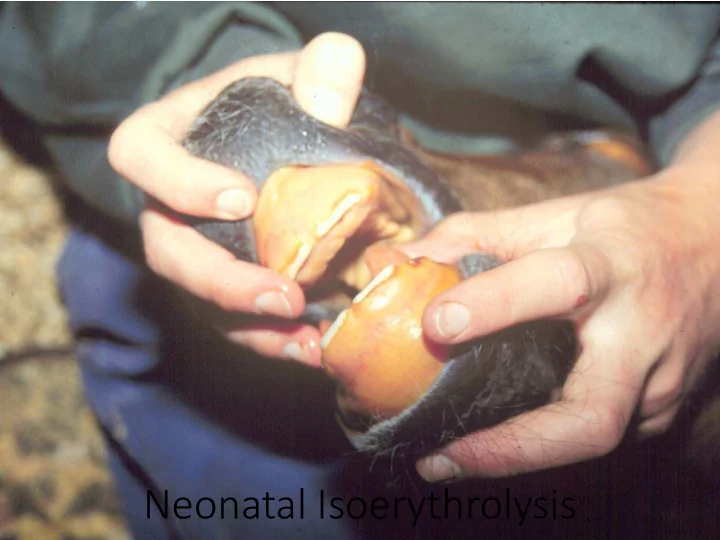
Neonatal Isoerythrolysis Neonatal Isoerythrolysis Pathogenesis - - PowerPoint PPT Presentation
Neonatal Isoerythrolysis Neonatal Isoerythrolysis Pathogenesis Immune mediated hemolytic anemia Mediated by maternal anti-RBC antibodies Colostrum Neonatal Isoerythrolysis Pathogenesis Foal inherits specific RBC Ag from the sire