FUNGAL INFECTION
Amanda Kozlik Chelsea Thompson Farbod Khaleghi Lisa D’Angelo Nestor Otero
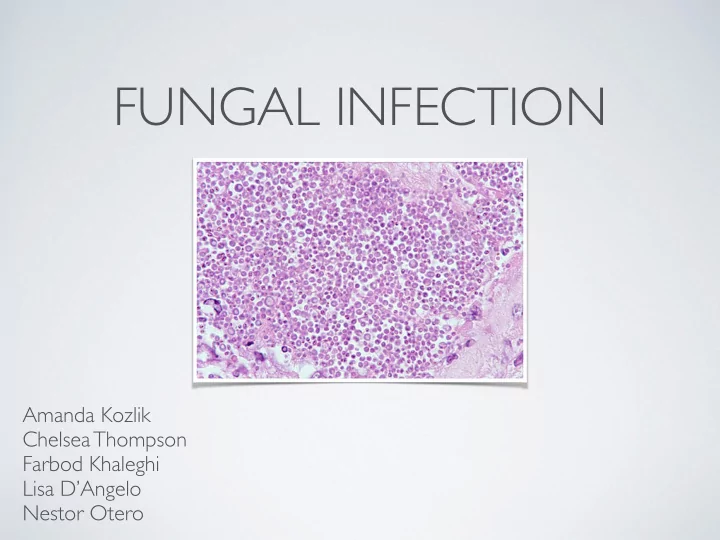
FUNGAL INFECTION Amanda Kozlik Chelsea Thompson Farbod Khaleghi - - PowerPoint PPT Presentation
FUNGAL INFECTION Amanda Kozlik Chelsea Thompson Farbod Khaleghi Lisa DAngelo Nestor Otero PATIENT PRESENTATION HPI: WM is a 66 y/o male who initially presented to the hospital for an upper GI bleed in September. The pt. had to be
Amanda Kozlik Chelsea Thompson Farbod Khaleghi Lisa D’Angelo Nestor Otero
hospital for an upper GI bleed in September. The pt. had to be intubated and his admission was complicated by concurrent Providencia stuarti pneumonia, esophagitis, intermittent fevers and the presence of yeast on a blood culture. He was seen by ID, treated for 2 wks for Candida glabrata fungemia and had his IJ Perm-A-Cath removed. He was discharged from the hospital off of all antibiotics/antifungals as he had completed his course of antibiotics and micafungin.
2
3
to esophagitis
pneumonia
fungemia
4
Tuesday
dialysis
PRN
5
SQ QHS
before meals
100-140, 5 units; 141-180, 6 units; 181-220, 7 units; 221-260, 8 units; 261-300, 9 units; 301-340, 10 units; > 341, call MD
be tachypneic, hypotensive and less responsive with a white count of 28.7, lactate of 3 and glucose level of 666.
lumbar puncture was not performed.
time of last admission (no significant changes since then)
6
the right groin femoral line, obtaining a TTE & additional ophthalmology exam and consulting pharmacy.
Candida glabrata
Gram Positive Cocci
7
8
Timeline of WBC Levels Timeline of Temperature
11/23: 12.9 11/17: 28.7 11/24: 11.4 11/25: 13.4
11/17 PM: 98.1°F 11/22 PM: 102°F 11/23 AM: 97.8°F
11/23 PM: 101.6°F 11/25 AM: 101.4°F
9
10
VS: T 101.4ºF, P 95, RR 18, BP 122/60, Ht. 66 in., Wt. 123 lb., O2 97% (RA) Gen: chronically ill, nontoxic, turns head to voice, in NAD HEENT: anicteric sclera, pale conjunctiva, dry mucus membranes CV: RRR Lungs: clear Abd: soft, NT, G-tube is in place Neuro: tracks with his eyes, turns to voice, does not follow any commands
11
12
13
14
15
16 Leon C, et al. Crit Care Med. 2006; 34: 730-737. Gupta A, et al. Indian J Crit Care Med. 2015; 19(3): 151-154.
3 → WM: 13,400/mm 3
17
18 Pappas PG, et al. Clin Infect Dis. 2009; 48(5): 503-535.
19 Pappas PG, et al. Clin Infect Dis. 2009; 48(5): 503-535.
20 Pappas PG, et al. Clin Infect Dis. 2009; 48(5): 503-535.
21 Pappas PG, et al. Clin Infect Dis. 2009; 48(5): 503-535.
22 Pappas PG, et al. Clin Infect Dis. 2007; 45(7): 883-893.
assigned in 1:1:1 ratio to receive one of the following interventions
23 Pappas PG, et al. Clin Infect Dis. 2007; 45(7): 883-893.
suggesting invasive Candidiasis
24 Pappas PG, et al. Clin Infect Dis. 2007; 45(7): 883-893.
25 Pappas PG, et al. Clin Infect Dis. 2007; 45(7): 883-893.
Groups Treatment Success Time to Negative Culture Micafungin 100 mg 76.4% 2 days Micafungin 150 mg 71.4% 3 days Caspofungin 72.3% 2 days
Most appropriate option: micafungin 100 mg IV once daily
26
27
28
29
30
31
32
33
34
35
36
37
38
39
40
blood culture and resolution of s/sx of candidemia
41
42
until stable
43
in critically ill patients. Indian J Crit Care Med. 2015; 19(3): 151-154.
, et al. A bedside scoring system (Candida score) for early anti fungal treatment in non-neutropenic critically ill patients with Candida colonization. Crit Care Med.2006; 34: 730-737.
Management of Candidiasis: 2009 Update by the Infectious Diseases Society
treatment of candidemia and other forms of invasive candidiasis. Clin Infect Dis. 2007; 45(7): 883-893.
44
45