Adverse Impacts of Severe ASCVD Is PCSK9 Inhibition the Key to Improving Patient Outcomes?
1
Adverse I m pacts of Severe ASCVD:
I s PCSK9 I nhibition the Key to I m proving Patient Outcom es?
Eliot A. Brinton, MD, FAHA, FNLA President, Utah Lipid Center Salt Lake City, Utah Past President, American Board of Clinical Lipidology
Educational Objectives
At the conclusion of this activity, participants should be able to:
- Evaluate the extent of residual CVD risk to which high-risk
patients are exposed
- Analyze the potential strengths and weaknesses of new
approaches to reduce CVD risk
- Incorporate insights about new LDL-lowering agents in
combination with statin therapy into more comprehensive clinical treatment strategies
- Discuss strategies to improve the knowledge, skills, or
performance of the healthcare team
Elevated LDL-C
Cardiovascular Pathobiology
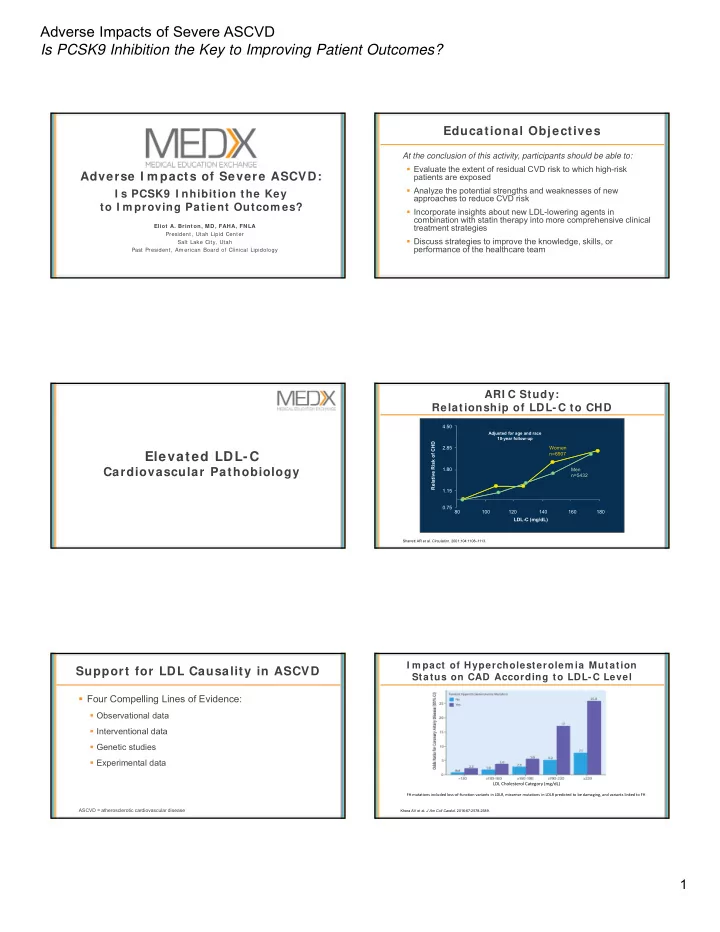
80 100 120 140 160 180 LDL-C (mg/dL) 4.50 2.85 1.80 1.15 0.75 Relative Risk of CHD Women n=6907 Men n=5432
Adjusted for age and race 10-year follow-up
ARI C Study: Relationship of LDL-C to CHD
Sharrett AR et al. Circulation. 2001;104:1108–1113.
Support for LDL Causality in ASCVD
- Four Compelling Lines of Evidence:
- Observational data
- Interventional data
- Genetic studies
- Experimental data
ASCVD = atherosclerotic cardiovascular disease
Khera AV et al. J Am Coll Cardiol. 2016;67:2578-2589.
I m pact of Hypercholesterolem ia Mutation Status on CAD According to LDL-C Level
FH mutations included loss‐of‐function variants in LDLR, missense mutations in LDLR predicted to be damaging, and variants linked to FH
LDL Cholesterol Category (mg/dL)