1
Lipid-Lowering Agents
Edward JN Ishac, Ph.D.
Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University Richmond, Virginia, USA Smith Building, Room 742 eishac@vcu.edu 828-2127
Agents used in the treatment of HT, CHF, Arrhythmia and Angina
Tolerance, flushing, dizziness, headache, reflex tachycardia aaa a aa Nitrates Effects enhanced in depolarized tissue, damaged tissue. Phase 0 aaa a Na+-Channel blockers Flushing, dizziness, headache, reflex tachycardia, combo Rx aa aaa Vasodilators Many Rx interactions, low TI, [K+] , important, low K+→↑toxicity a aa Cardiac glycosides Low GFR, hypokalemia → CG; glucose intolerance → diabetes aaa a aaa a Diuretics Low GFR, renal stenosis, glossitis, tetrogenic, cough (ACEI), taste, ↑renal mechanics aaa a aaa a ACEI / ARBs CHF, Gingival hyperplasia, reflex tachycardia, constipation aaa a aaa a aaa a Ca++-Channel blockers Caution: CHF (unstable CHF, bronchospasm, significant bradycardia); or in diabetes, asthma (use β1-selective), depression aaa a aaa aaa aaa a Beta-Blockers Contraindications/Cautions/Notes Angina Arrhyth mia CHF Hyper- tension Drug Class
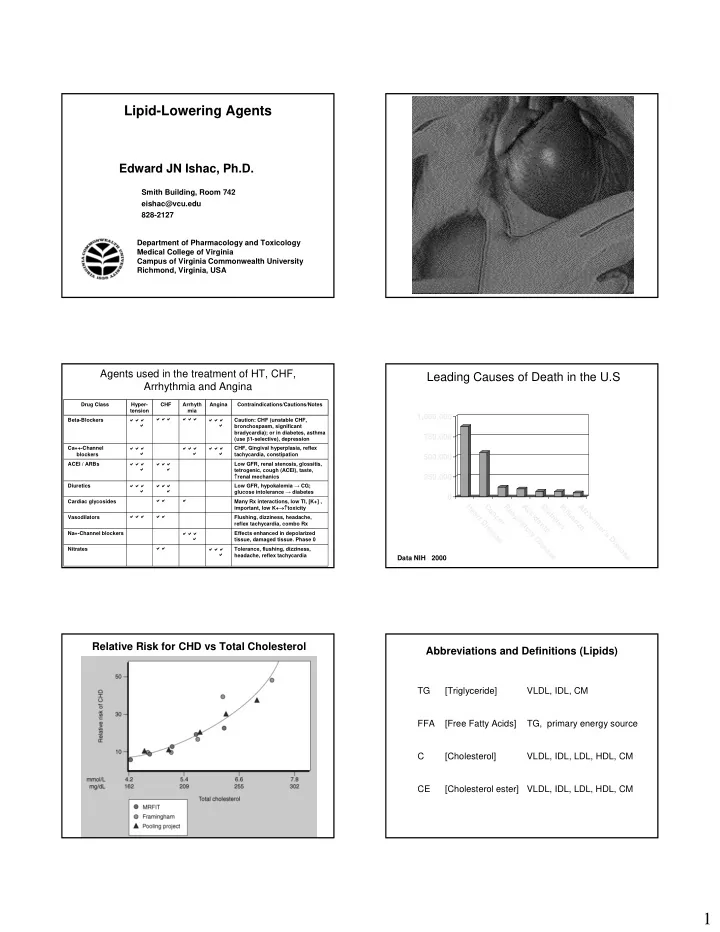
Leading Causes of Death in the U.S
250,000 500,000 750,000 1,000,000 H e a r t D i s e a s e C a n c e r R e s p i r a t
- r
y D i s e a s e A c c i d e n t s D i a b e t e s I n f l u e n z a A l z h e i m e r ' s D i s e a s e
Data NIH 2000