4/17/2015 1
UCSF Vascular Symposium 2015 Presentation
CONTROVERSIES IN DIALYSIS ACCESS
- DR. JOHN R. ROSS
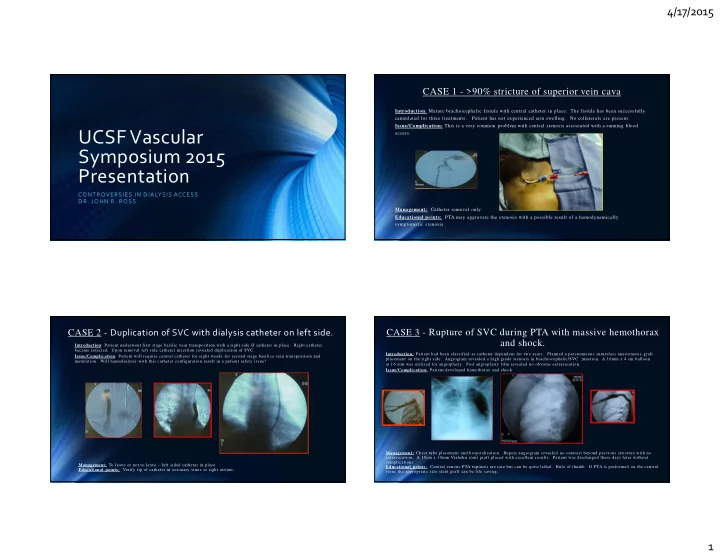
CASE 1 - >90% stricture of superior vein cava
Introduction: Mature brachiocephalic fistula with central catheter in place. The fistula has been successfully cannulated for three treatments. Patient has not experienced arm swelling. No collaterals are present. Issue/Complication: This is a very common problem with central stenosis associated with a running blood access. Management: Catheter removal only. Educational points: PTA may aggravate the stenosis with a possible result of a hemodynamically symptomatic stenosis.
CASE 2 - Duplication of SVC with dialysis catheter on left side.
Introduction: Patient underwent first stage basilic vein transposition with a right side IJ catheter in place. Right catheter became infected. Upon removal left side catheter insertion revealed duplication of SVC. Issue/Complication: Patient will require central catheter for eight weeks for second stage basilica vein transposition and
- maturation. Will hemodialysis with this catheter configuration result in a patient safety issue?
Management: To leave or not to leave – left sided catheter in place Educational points: Verify tip of catheter in coronary sinus or right atrium.
CASE 3 - Rupture of SVC during PTA with massive hemothorax and shock.
Introduction: Patient had been classified as catheter dependent for two years. Planned a percutaneous sutureless anastomosis graft placement on the right side. Angiogram revealed a high grade stenosis in brachiocephalic/SVC junction. A 10mm x 4 cm balloon at 16 atm was utilized for angioplasty. Post angioplasty film revealed no obvious extravasation. Issue/Complication: Patient developed hemothorax and shock. Management: Chest tube placement and hospitalization. Repeat angiogram revealed no contrast beyond previous stricture with no
- extravasation. A 10cm x 10mm Viabahn stent graft placed with excellent results. Patient was discharged three days later without
complications. Educational points: Central venous PTA ruptures are rare but can be quite lethal. Rule of thumb: If PTA is performed on the central veins the appropriate size stent graft can be life saving.