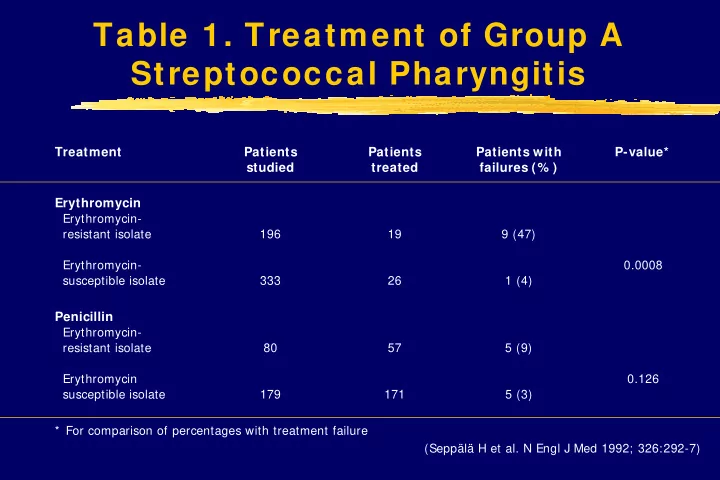
Table 1. Treatment of Group A Streptococcal Pharyngitis
Treatment Patients studied Patients treated Patients with failures (% ) P-value* Erythromycin
Erythromycin- resistant isolate 196 19 9 (47) Erythromycin- susceptible isolate 333 26 1 (4) 0.0008
Penicillin
Erythromycin- resistant isolate 80 57 5 (9) Erythromycin susceptible isolate 179 171 5 (3) 0.126 * For comparison of percentages with treatment failure (Seppälä H et al. N Engl J Med 1992; 326:292-7)