Sunscreens, Spots and Skin Cancer Common lesions Skin cancers - PDF document
Outline Sunscreens, Spots and Skin Cancer Common lesions Skin cancers Lindy P. Fox, MD Non melanoma Professor of Clinical Dermatology Director, Hospital Consultation Service Melanoma Department of Dermatology University of
Outline Sunscreens, Spots and Skin Cancer • Common lesions • Skin cancers Lindy P. Fox, MD – Non‐ melanoma Professor of Clinical Dermatology Director, Hospital Consultation Service – Melanoma Department of Dermatology University of California, San Francisco • Sunscreen lindy.fox@ucsf.edu I have no conflicts of interest to disclose I may be discussing off-label use of medications 1 Common Skin Lesions Seborrheic Keratoses • Seborrheic keratosis • BENIGN • Dermatofibroma • Appear beginning at age 40, earlier in • Cherry angioma sunny regions • Stuck-on morphology (above the skin) • Pyogenic granuloma • Greasy/waxy/warty texture, horn cysts • Chondrodermatitis nodularis helices • Face, under breasts, trunk • Sebaceous hyperplasia • 0.1 to 2.0 cm in diameter • Treatment: Reassure, cryotherapy
Dermatofibroma • Firm, 3‐7 mm slightly rough surfaced, slightly elevated papules • Overlying hyperpigmentation • Firm to palpation; Dimple sign • Often at sites of minimal trauma – Bug bite, ingrown hair, etc • Treatment : Reassure, cryotherapy, removal • Often recur after removal • Association: Multiple (>15) of sudden onset may rarely signal T cell dysregulation (Lupus, HIV) Cherry Angioma • Very Common • Increases with age (senile angioma) • F>M (?hormonal) • 1‐5 mm bright red dome‐shaped papule • Not easily compressible • Association: None • Complications: None
Pyogenic Granuloma • Friable, 5‐10 mm papule • Occurs after trauma • Children and adults • Biopsy: Excess granulation tissue • Treatment: Surgical removal (curette), electrodesiccation of base, topical timolol? • Complication: Rarely may recur and form satellites Chondrodermatitis Nodularis Helices • Benign nflammation of the cartilage of the helix or antihelix • Middle aged men • Painful! • “can’t sleep on that side” • May mimic NMSC • Treatment – Relieve pressure, surgical removal, time – LN2, IL kenalog, laser therapy
“CNH pillow” Sebaceous Hyperplasia • Common, benign • Single or multiple pink to yellow papules on the face, often with telangiectasias and central dell • May mimic BCC • Multiple associated with calcineurin inhibitors • When associated with sebaceous adenoma or sebaceous carcinoma, rule‐out Muir Torre (Lynch) syndrome • Treatment‐ low dose isotretinoin, electrodesiccation, laser, shave removal, PDT, cryotherapy Nonmelanoma Skin Cancer (NMSC) • Actinic Keratosis • Basal Cell Carcinoma • Squamous Cell Carcinoma • Caused primarily by ultraviolet radiation • SCC and Actinic Keratoses – P53 tumor suppression gene mutated by UV • BCC – PTCH gene
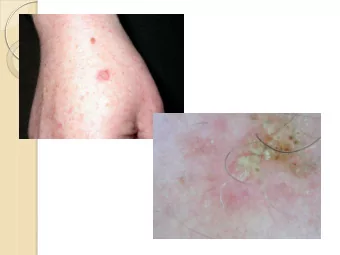
Actinic Keratosis Actinic Keratosis • In-situ dysplasia from ultraviolet exposure. • Diagnosis ‐ Clinical • Sign of sufficient sun injury to develop NMSC. inspection • • Precancerous (low rate <1%) Red, scaly patch < 6mm. • • Prevented by sun screen use, even in adults. Tender to touch. • Sandpaper consistency. • Location ‐ Scalp, face, dorsal hands, lower legs (women) • When very thick, suspect hypertrophic AK or SCC
Actinic Keratoses and SCC Actinic Keratoses Actinic Keratoses- Treatment Actinic Keratoses‐ Treatment • Liquid nitrogen (single freeze‐thaw cycle) • Always biopsy if an AK is not responding • Topical treatment • 5‐fluorouracil (0.5‐5%) (Efudex) to appropriate therapy • 5% qd or BID for 2‐4 weeks • Imiquimod 5% cream (Aldara) – r/o SCC, superficial BCC • TIW x 4 weeks, with repeated cycles PRN • BIW or TIW x 16 weeks • QW x 24 weeks • Diclofenac (Solareze) • BID x 60‐90 days • Long term treatment (>120 days), moderately effective, side effects • Ingenol mebutate (Picato); 0.015%, 0.05% • Face/scalp‐ 0.015% QD x 3d • Trunk/extrem‐ 0.05% QD x 2d • Photodynamic therapy
Basal Cell Carcinoma Basal Cell Carcinoma‐ Clinical Subtypes • Most common of all cancers • Nodular (classic) – > 1,000,000 diagnosed annually in USA • Superficial – Lifetime risk for Caucasians: up to 50% • Pigmented • Intermittent intense sun exposure and • Morpheaform (scar‐like) overexposure (sunburns) • Locally aggressive, very rarely • Clinical subtypes have different biologic metastasize behavior • Histologic subtypes also influence behavior Basal Cell Carcinoma‐ Nodular
Basal Cell Carcinoma‐ Superficial Basal Cell Carcinoma‐ Pigmented • Clinically pink, slightly scaly, slightly shiny • May be entirely pigmented or there may patch be specks of pigment within what otherwise looks like a nodular or • Looks like an actinic keratosis superficial BCC • May be treated with imiquimod, ED+C • Melanoma is on the differential!! Basal Cell Carcinoma‐ Morpheaform • Clinically scar-like • Difficult to determine clinically where lesion begins and ends • Treat with excision (have pathologist check margins) or Mohs micrographic surgery – DO NOT ED+C
Basal Cell Carcinoma‐ Treatment Location, Size, and Subtype Guide Therapy • Superficial • Imiquimod • Electrodesiccation and curettage (ED+C) • Nodular or pigmented • ED+C • Excision (4mm margins) • Mohs micrographic surgery • Radiation‐ comorbidities, tumor size and location • Morpheaform, infiltrative, micronodular • Excision (4mm margins) • Mohs micrographic surgery J Am Acad Dermatol 2018;78:540-59 Topical Treatment of Skin Cancer Topical Treatment of Skin Cancer • Patient selection is the key • Scarring may be reduced compared to surgery • Work for superficial cancers (NOT invasive ones) • Superficial BCC ’ s and SCC in situ • Superficial BCC, SCC in situ • Long courses (months) may be required • Imiquimod 5% cream • – 5X per week for 6-10 weeks depending on the host Biopsy to confirm diagnosis before reaction treating – Efficacy 75%-85% • 5FU- – Topically twice daily for up to 12 weeks
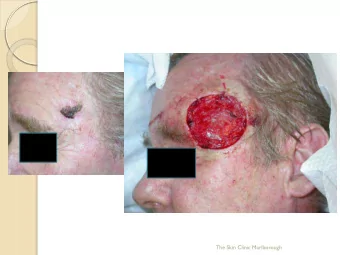
Basal Cell Carcinoma‐ Treatment Squamous Cell Carcinoma Mohs micrographic surgery • Presents as red • Recurrent or incompletely excised tumors plaque, ulceration, or • Aggressive histologic subtype (infiltrative, wart like lesion morpheaform, micronodular) • Risk factors: • Poorly defined clinical margins – Fair skin • High risk location (face, ears, eyes) – Inability to tan – Chronic sun exposure • Large (>1.0 cm face, >2.0 cm trunk, extrem) • Special situations: • Tissue sparing location (face, hands, genitalia) – Organ transplant • Immunosuppressed patients recipients • Tumors in previously irradiated skin or scar • Tumors arising in setting of genetic diseases Keratoacanthoma • Rapidly growing (1month) • Dome-shaped nodule with central core of keratin • May spontaneously regress, but treat as an SCC
Squamous Cell Carcinoma Treatment • SCC in situ – 5-FU – Imiquimod – Liquid nitrogen – Electrodesiccation and curettage • Invasive SCC – Excision with 4-6 mm margins – Mohs micrographic surgery J Am Acad Dermatol 2018;78:560-78 J Am Acad Dermatol 2018;78:560-78 Squamous Cell Carcinoma‐ Treatment Skin Cancers on the Lower Legs Mohs micrographic surgery • • BCC and SCC in situ is common on the Recurrent or incompletely excised tumors • lower legs, especially in women Aggressive histologic subtype (perivascular, perineural) • Poorly defined clinical margins • Fixed, red, scaly patch(es) • High risk location (face, ears, eyes) – Mimic eczema • Large (>1.0 cm face, >2.0 cm trunk, extrem) • Think of skin cancer when red patches on • Tissue sparing location (face, hands, genitalia) the lower legs don ’ t clear with • Immunosuppressed patients moisturizing. • Tumors in previously irradiated skin or scar • Tumors arising in setting of genetic diseases
Case • 64M with psoriasis, hypertension, s/p renal transplant • Ulcer x 3 months of ulceration, thought to be due to venous insufficiency • 3 months of topical treatment fails to improve ulceration Skin Cancer in Organ Transplant Recipients • Skin Biopsy = Squamous • Skin cancer is most common malignancy in OTR Cell Carcinoma • Incidence increases with survival time post • Chronic phototherapy and transplant immunosuppressive • 90% are nonmelanoma skin cancer: SCC>BCC treatments have led to skin – Squamous cell carcinoma (SCC) cancer • 65 X the incidence in the general population • If leg ulcer doesn ’ t heal with – Basal cell carcinoma appropriate treatment—refer • 10 X the incidence in the general population or biopsy
Acquired Nevi (Moles) Skin Cancer in Organ Transplant Recipients • Biologic behavior much more aggressive than in the • Almost universal general population • Risk Factors • In areas of sun exposure – Older age • Change throughout life, appearing at preschool – Increased exposure to UV radiation age, growing during young adulthood, and – Increased immunosuppression involuting in old age – Fair skin • 5mm in diameter or less (size of pencil eraser) – Personal history of AK, NMSC, melanoma – Heart > kidney > liver transplants • Size (>6mm), number (more than 50) and pattern – HPV infection (not in sun exposed sites) predicts melanoma – Voriconazole • Refer OTR to a dermatologist for regular skin checks Atypical Moles • Not in sun exposed sites • Larger than 6 mm in diameter • Greater than 50
Recommend
More recommend
Explore More Topics
Stay informed with curated content and fresh updates.