4/8/2017 1
The Plastic Surgeons Role on the Limb Salvage Team
Scott L. Hansen, M.D., F.A.C.S Associate Professor of Surgery University of California, San Francisco
Limb Salvage
Hansen 2017 Hansen 2017
Complex Lower Extremity Injuries
Hansen 2017
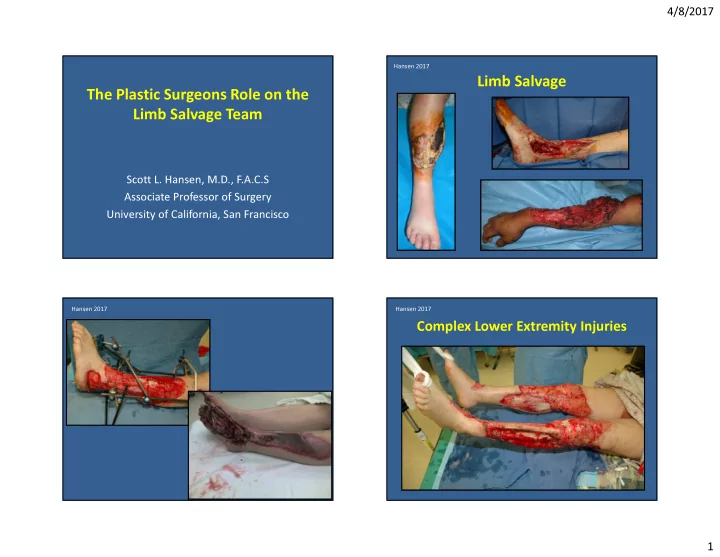
Limb Salvage The Plastic Surgeons Role on the Limb Salvage Team - - PowerPoint PPT Presentation
4/8/2017 Hansen 2017 Limb Salvage The Plastic Surgeons Role on the Limb Salvage Team Scott L. Hansen, M.D., F.A.C.S Associate Professor of Surgery University of California, San Francisco Hansen 2017 Hansen 2017 Complex Lower Extremity
Hansen 2017 Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017 Hansen 2017
Hansen 2017 Hansen 2017
Hansen 2017 Hansen 2017 Hansen 2017
Hansen 2017
Hansen 2017 Hansen 2017 Hansen 2017 Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017 Ian Taylor, MD
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017 Hansen 2017 Hansen 2017 Hansen 2017
Hansen 2017
Hansen 2017 Hansen 2017 Hansen 2017
Hansen 2017 Hansen 2017 Hansen 2017 Hansen 2017
Hansen 2017 Hansen 2017 Hansen 2017
Hansen 2017
Hansen 2017 Hansen 2017 Hansen 2017
Hansen 2017
62
Hansen 2017
Hansen SL. Flaps, Plastic Surgery, Mathes SJ, Hentz VR (eds), Saunders and Co., New York 2005.
Hansen 2017
Muscle vs. fasciocutaneous flap coverage
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017
Hansen 2017