Darwin Chen, MD Assistant Professor Mount Sinai Medical Center Department of Orthopaedic Surgery
Femoral Bone Loss in Revision THA Darwin Chen, MD Assistant - - PowerPoint PPT Presentation
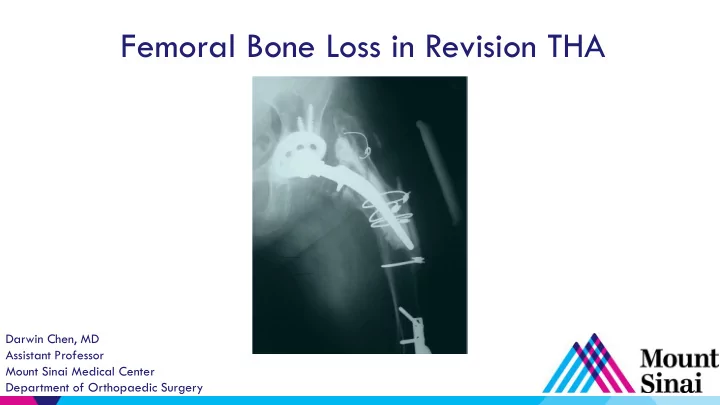
Femoral Bone Loss in Revision THA Darwin Chen, MD Assistant - - PowerPoint PPT Presentation
Femoral Bone Loss in Revision THA Darwin Chen, MD Assistant Professor Mount Sinai Medical Center Department of Orthopaedic Surgery Disclosures Monogram Orthopedics Consultant The Challenge of Femoral Revision Proximal femoral
▶ Monogram Orthopedics
– Consultant
Disclosures
The Challenge of Femoral Revision
▶ Proximal femoral bone loss
– Osteolysis – Stress shielding – Implant removal – ETO
▶ Loose stems - varus and retroverted femoral
remodeling
▶ Goal: Stable distal fixation and
preservation of bone stock
Paprosky Classification
▶ Reliable, reproducible ▶ Predicts intraoperative bone loss ▶ Quantifies remaining femoral host bone ▶ Guides reconstructive options ▶ Can easily turn a I/II into a III with iatrogenic
damage!
Paprosky I
▶ Minimal metaphyseal
bone loss
▶ Diaphysis intact ▶ Tx: standard stem
– Cementless or cemented
Paprosky I
Paprosky I
Paprosky II
▶ Metaphysis damaged, non-
supportive
▶ Isthmus fully intact ▶ Diaphyseal cortices supportive ▶ Tx – diaphyseal engaging
stem, +/- proximally fixed
Paprosky II
▶ Proximally coated, distally fixed - SROM
Paprosky II
▶ Diaphyseal engaging – modular tapered Ti
Paprosky III (A vs. B)
▶ Metaphysis is severely damaged
and non-supportive
▶ Diaphysis intact
– 3A >4cm of isthmus – 3B <4cm
▶ Diaphyseal fixation ▶ Tx: 3A - fully coated cylindrical
3B – tapered fluted (Wagner)
Paprosky IIIA
▶ >4cm isthmus - fully coat cylindrical
Paprosky IIIA
Paprosky IIIB
▶ <4cm isthmus - tapered fluted Ti
– Monobloc (Wagner type) vs. modular
Paprosky IV
▶ Extensive meta-diaphyseal
damage
▶ Nonsupportive isthmus ▶ Analogous to Vancouver B3 ▶ Tx
– Megaprosthesis – APC – Tapered fluted Ti Stem?
Paprosky IV
▶ Megaprosthesis
– Salvage
Extended Trochanteric Osteotomy (ETO)
▶ Facilitates
– Exposure – Component/cement removal – Reaming/insertion of revision stem
~12-15cm
The Workhorse: Modular Tapered Ti Stem
▶ Applicable for almost every revision
case (Type 1-3b, some 4s)
▶ Reliable, reproducible, simple
– New gold standard?
▶ “Pot” the distal stem where it wants to
go
▶ “Build” up with the proximal body –
Length, offset, version, proximal fill
Not All Modular Tapered Stems Are Created Equal!
▶ Taper angle
– Axial stability – 2 to 3.5 degrees
▶ Spline design
– Rotational stability – Sharp/flat/variable
▶ Distal geometry
– Kinked/bowed/beveled
Not All Modular Tapered Stems Are Created Equal!
▶ Modular junction problems
– Breakage – Corrosion?
▶ Subsidence ▶ Cost
What is the Limit of a Modular Tapered Stem?
▶ B/l loose hemis, severe varus remodeling (R cemented, infected)
What is the Limit of a Modular Tapered Stem?
▶ Vancouver B3 periprosthetic fx / Paprosky IV (1cm isthmus left)
Technique Tips – Mod Tapers
▶ ETO for implant removal or
varus remodeling
▶ Distal prophylactic cable if ETO
- r any doubt
▶ Ream on power vs hand? ▶ Ream to a mid size proximal
modular body
▶ Low threshold for intraop XR
Technique Tips – Mod Tapers
▶ Be wary of anterior distal stem perforation
Technique Tips – Mod Tapers
▶ Make sure to bottom out the proximal body reamer
Conclusions
▶ Diaphyseal fixation is key for femoral revisions ▶ ETO for safe implant removal, deformity correction, and easier
reaming
▶ Modular tapered Ti stems are the workhorse for most revisions ▶ “Pot” and “build” ▶ Be watchful for subsidence, perforation, junctional failures
Thank You
Darwin Chen, MD Assistant Professor Mount Sinai Medical Center Department of Orthopaedic Surgery