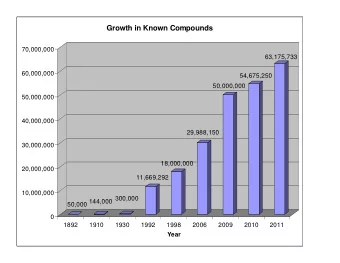
175,000 Australians live with chronic HCV infection (December 2017) - PowerPoint PPT Presentation
An eHealth model of care for the community and prison treatment of chronic hepatitis C Dr James Haridy BPhysio MBBS MPH (Nutrition) CHIA FRACP Gastroenterologist & Hepatologist, PhD Candidate @jamesharidy University of Melbourne, Royal
An eHealth model of care for the community and prison treatment of chronic hepatitis C Dr James Haridy BPhysio MBBS MPH (Nutrition) CHIA FRACP Gastroenterologist & Hepatologist, PhD Candidate @jamesharidy University of Melbourne, Royal Melbourne Hospital
175,000 Australians live with chronic HCV infection (December 2017) Stigma Symptoms
Uptake of new hepatitis medications in Australia over the first 18-months Source: The Kirby Institute, Sydney(2) Screened Confirmed HCV Ab + Cured 83% 33%
Hepatitis C is easily curable with new treatments. Elimination is possible. Treatment needs to take place in the community in order to reach everybody who needs it The Declining treatment rate and most community clinicians have not prescribed these new treatments problem Followup in community settings to check for cure and other liver problems is an issue Current methods to support GPs/nurses are slow, rely on fax, do not offer ongoing support
GP NURSE PRACTITIONER
Prospective Studies An eHealth model of care for the community and prison treatment of hepatitis C
What is the ‘eHealth model’? GP PRACTICE NURSE HEPATITIS NURSE SPECIALIST PATIENT This study aims to compare the use of an online shared care system for treating hepatitis C compared to the current standard of care using the remote consultation form
What is the ‘eHealth model’? Four main components Potential Benefits: Potential Benefits: Potential Benefits: Potential Benefits: 3. Electronic Patient Portal 4. Shared Disease Record 1. Clinical Decision Support System Increase ease of prescribing Database to allow follow-up Involves patient in treatment Allow direct link with specialist 2. Electronic Messaging Overcome unfamiliarity with drugs Remote monitoring from specialist teams Direct line of communication for followup Referral of treatment plans Increase adherence to guidelines
Methods Quasi experimental, prospective pre-post study Arm 1: Community Arm 2: Prison All patients intended for All patients intended for HCV treatment by HCV treatment by prison enrolled GPs and nurses medical officers without without physical specialist physical specialist review review Compared to community and prison cohort managed via remote consultation (paper, fax, phone) March 1 st 2016 – February 28 th 2017
Efficacy (SVR12) - Primary Outcome Acceptability Questionnaire, interviews Usability System Usability Scale, Interview, Usability Testing Uptake, Utilisation and Demand Outcomes Usage of doctor, nurse and patient portal Integration & Implementation Questionnaire, feedback and semi-structured interviews Quality & Safety Adherence to guideline, optimal treatment selection Efficiency Time per referral, Turnaround time for approval
Recruitment 61 GPs 2 PRISONS 9 HEPATITIS 8 PRACTICE 13 SPECIALISTS 3 medical officers, 7 prison nurses NURSES NURSES 8 Tertiary Hospitals Pre-intervention group 273 PATIENTS 588 community treatments 84 prison treatments
273 PATIENTS COMMUNITY ARM (n=201) PRISON ARM (n=72) Excluded (n=28): Excluded (n=10): Referral Rejected (n=1) Draft plan only (n=10) Draft plan only (n=27) Treatment plan initiated Treatment plan initiated (n=173) (n=62) Treatment in progress (n=46) Treatment in progress (n=140) Completed Completed (n=33) (n=16)
Patient Characteristics Control HealthElink (n=588) (n=273) Age, years, median (IQR # ) 48 (40-56) 46 (38-54) Sex, male, n (%) 400 (68.0%) 204 (74.7%) ATSI * , n (%) 17 (4.3%) 30 (11.0%) Patient Residence (ARIA ## Score) Major City, n (%) 329 (57.6%) 169 (61.9%) Inner Regional n (%) 156 (27.3%) 13 (4.8%) Outer Regional n (%) 42 (8.2%) 84 (30.8%) Remote n (%) 34 (7.4%) 5 (1.8%) Very Remote n (%) 10 (0.3%) 2 (0.7%) Medical History HIV, n (%) 4 (0.7%) 1 (0.4%) Study HBV, n (%) 1 (0.2%) 3 (1.1%) Diabetes, n (%) 19 (3.5%) 14 (5.2%) Obesity, n (%) 30 (14.2%) 23 (8.7%) ETOH, >50g daily, n (%) 25 (12.0%) 56 (20.6%) Cirrhosis, n (%) 30 (5.4%) 41 (18.0%) Population Opioid Substitution Therapy, n (%) 80 (31.6%) 33 (12.1%) PWID, current, n (%) N/A 22 (8.1%) PWID, ex, n (%) N/A 125 (45.8%) Primary treating clinician Nurse-led treatment, n (%) 141 (24.0%) 159 (79.1%) General practitioner-led treatment, n (%) 447 (76.0%) 42 (20.9%) Hepatitis C Assessment Treatment experienced, n (%) 40 (8.1%) 18 (7.9%) Genotype 1a, n (%) 262 (44.6%) 97 (37.3%) Genotype 1b, n (%) 40 (6.8%) 21 (8.1%) Genotype 1 not specified, n (%) 5 (0.9%) 0 (0%) Genotype 2, n (%) 22 (3.7%) 12 (4.6%) Genotype 3, n (%) 257 (43.8%) 118 (45.4%) Genotype 4, n (%) 1 (0.2%) 3 (1.2%) Genotype 6, n (%) 0 (0%) 9 (3.5%)
Interim Outcomes 49/236 (21%) of outcomes collected in interim analysis Intention to Treat SVR12% 100 89% 88% HealthElink 80% 80 74% Control 71% 62% SVR12 % 60 40 20 4 279 25 104 14 62 5 447 28 141 16 87 0 GP Nurse Prison Community
Interim Outcomes Liver Biochemistry Treatment to National Guideline 100% 98.6% 100 96% 100 80 80 Completion % Completion % 56% 60 60 40 40 251 656 20 44 372 20 251 665 46 665 0 0 HealthEl Control HealthEl Control
Interim Outcomes Patient Portal Usage 23/61 GPs have entered at least one patient on 250 201 the system 200 number (n) 150 100 50 All specialists and hepatitis 23 5 nurses have utilised the 0 Total Eligible Registered system
Enablers, barriers and experience Highest uptake and early Early issues with positive feedback from integration across web ‘closed’ systems such as browsers and internet prison/hepatitis nurses. access in some areas Double data entry a Data management - barrier (even if it takes the assessments not available same time as the paper- in the control group based form) Notifications utilising Uptake appears highest in email have been areas where value is problematic perceived (prisons, rural)
Thankyou @jamesharidy Supervisors Disclosures and Grants Dr Edmund Tse - Royal Adelaide/Darwin Hospitals RMH Foundation Dr Guru Iyngkaran – Royal Melbourne/Darwin Hospitals MSD (Grant, Speaker Fees) A/Prof Amanda Nicoll - Eastern Health BMS (Grant, Speaker Fees) A/Prof Geoff Hebbard - Royal Melbourne Hospital Collaborators & Investigators Dr Niranjan Ararachi - Western Health Dr Renjy Nelson - Queen Elizabeth Hospital Dr Rod Omond – Top End Primary Care Ms Rachel Liddle - Western Health Dr Dep Huynh – Queen Elizabeth Hospital Dr Catherine Marshall – Royal Darwin Hospital Dr Kate Muller - Flinders Medical Centre Mr Jeffrey Stewart - Queen Elizabeth Hospital Dr Jane Davies - Royal Darwin Hospital Ms Rosalie Altus - Flinders Medical Centre Ms Jaclyn Tate-Baker - Royal Darwin Hospital Dr Suresh Sivanesan - Royal Melbourne Hospital Mr Anton Colman - Royal Adelaide Hospital Dr Tim Fazio - Royal Melbourne Hospital Prof Meredith Temple-Smith – University of Melbourne Dr Dep Huynh - Queen Elizabeth Hospital Ms Sally Watkinson - Royal Melbourne Hospital Dr Mark Wilson - Royal Hobart Hospital Dr Zina Valaydon – Western Health Prof Alan Wigg – Flinders Medical Centre Dr Stephen Bloom - Eastern Health Dr Jeyamani Ramachandran – Flinders Medical Centre Professor Danny Liew – Monash University A/Prof John Lubel - Eastern Health www.healthelinkstudy.com.au
Recommend
More recommend
Explore More Topics
Stay informed with curated content and fresh updates.