- - First shoulder arthroplasty
Reverse Total Shoulder Arthroplasty
James H. Chang May 3, 2007 UCSD
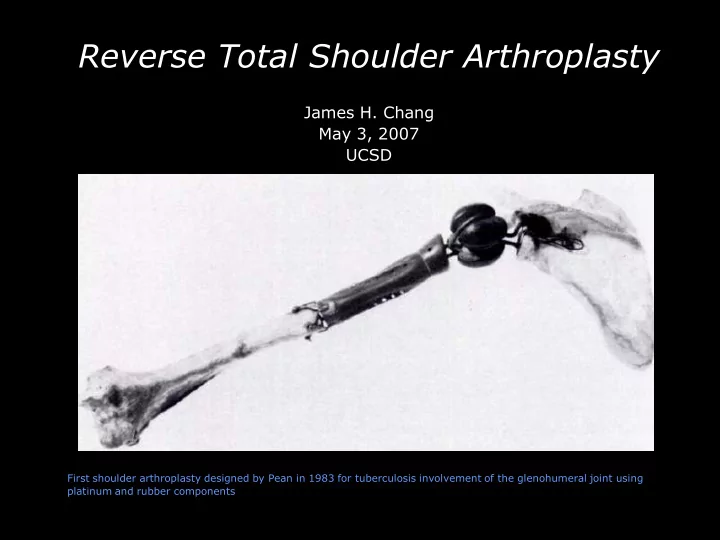
First shoulder arthroplasty designed by Pean in 1983 for tuberculosis involvement of the glenohumeral joint using platinum and rubber components
Reverse Total Shoulder Arthroplasty James H. Chang -- First - - PowerPoint PPT Presentation
Reverse Total Shoulder Arthroplasty James H. Chang -- First shoulder arthroplasty May 3, 2007 UCSD First shoulder arthroplasty designed by Pean in 1983 for tuberculosis involvement of the glenohumeral joint using platinum and rubber components
First shoulder arthroplasty designed by Pean in 1983 for tuberculosis involvement of the glenohumeral joint using platinum and rubber components
Conventional TSA not satisfactory
Unconstrained TSA abandoned b/c of glenoid loosening
Courtesy Tudor Hughes, M.D.
Courtesy Heinz Hoenecke, M.D.
Unconstrained TSA abandoned b/c of glenoid loosening
Unconstrained TSA abandoned b/c of glenoid loosening
Glenoid baseplate not fully seated
Component loosening
Courtesy Heinz Hoenecke, M.D.
Scapular Notching
Scapular Notching
Malpositioning of metaglene screw
Acromial Stress Fracture
Scapular spine fracture
Courtesy Heinz Hoenecke, M.D.
END