Emergency series
Dr Shuaib Siddiqui, MB BChir MRCP, FY3 doctor
Content reviewed on 12/05/2020.
Quiz
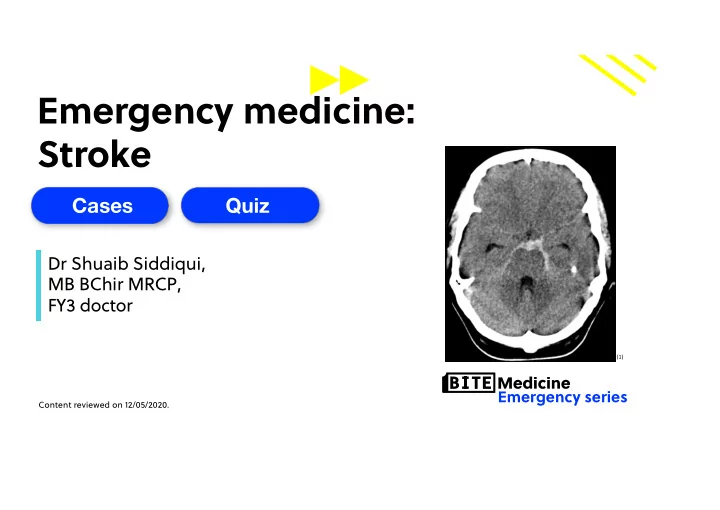
Emergency medicine: Stroke
Cases Quiz
(1)
Emergency medicine: Stroke Cases Quiz Quiz Dr Shuaib Siddiqui, - - PowerPoint PPT Presentation
Emergency medicine: Stroke Cases Quiz Quiz Dr Shuaib Siddiqui, MB BChir MRCP, FY3 doctor (1) Emergency series Content reviewed on 12/05/2020. Case 1 History You are working in A&E. You see a 70-year-old man who is brought in by
Emergency series
Dr Shuaib Siddiqui, MB BChir MRCP, FY3 doctor
Content reviewed on 12/05/2020.
Quiz
(1)
History You are working in A&E. You see a 70-year-old man who is brought in by ambulance after his son noticed he was slurring his speech. This started 3 hours ago. On examination, you note he has 3/5 power of both his left upper limb and 4/5 power of his left lower limb. Observations HR 90, BP 155/89 mmHg, RR 18, SpO2 97%, Temp 36.8
2
3
History You are working in A&E. You see a 70-year-old man who is brought in by ambulance after his son noticed he was slurring his speech. This started 3 hours ago. On examination, you note he has 3/5 power of both his left upper limb and 4/5 power of his left lower limb. Observations HR 90, BP 155/89 mmHg, RR 18, SpO2 97%, Temp 36.8
4
5
6
Definition: sudden onset of rapidly developing focal or global neurological disturbance which lasts more than 24 hours or leads to death (NICE)
Ischaemic (85%) Thrombotic
Embolic
Lacunar
Hypoperfusion
Haemorrhagic (15%) Intracerebral
Subarachnoid
7
Definition: sudden onset of rapidly developing focal or global neurological disturbance which lasts more than 24 hours or leads to death (NICE) Epidemiology
Risk factors
8
Stroke TIA Definition Sudden onset of rapidly developing focal or global neurological disturbance which lasts more than 24 hours or leads to death Transient neurological symptoms lasting less than 24 hours
9
Stroke TIA Definition Sudden onset of rapidly developing focal or global neurological disturbance which lasts more than 24 hours or leads to death Transient episode of neurological dysfunction caused by focal brain, spinal cord, or retinal ischaemia, without acute infarction Imaging Infarction No infarction Tissue Hypoxic damage No changes
10
History You are working in A&E. You see a 70-year-old man who is brought in by ambulance after his son noticed he was slurring his speech. This started 3 hours ago. On examination, you note he has 3/5 power of both his left upper limb and 4/5 power of his left lower limb. Observations HR 90, BP 155/89 mmHg, RR 18, SpO2 97%, Temp 36.8
11
History You are working in A&E. You see a 70-year-old man who is brought in by ambulance after his son noticed he was slurring his speech. This started 3 hours ago. On examination, you note he has 3/5 power of both his left upper limb and 4/5 power of his left lower limb. Observations HR 90, BP 155/89 mmHg, RR 18, SpO2 97%, Temp 36.8
12
(2)
13
(3)
14
Territory Signs
Anterior cerebral artery Contralateral hemiparesis and sensory loss
Middle cerebral artery Contralateral hemiparesis and sensory loss
Contralateral homonymous hemianopia Aphasia (dominant hemisphere) Hemispatial neglect (non-dominant hemisphere)
15
(4)
16
Hemispheric dominance
(5) (6)
17
Hemispheric dominance
(7)
18
19
Territory Signs
Posterior cerebral artery
infarction Vertebrobasilar artery
20
(8) (6)
21
22
(6)
23
Feature Score
Loss of consciousness or syncope
Seizure activity
New, acute onset: Asymmetric facial weakness + 1 point Asymmetric arm weakness + 1 point Asymmetric leg weakness + 1 point Speech disturbance + 1 point Visual field defect + 1 point
24
Bedside
Bloods
Imaging
25
History You are working in A&E. You see a 70-year-old man who is brought in by ambulance after his son noticed he was slurring his speech. This started 3 hours ago. On examination, you note he has 3/5 power of both his left upper limb and 4/5 power of his left lower limb. Observations HR 90, BP 155/89 mmHg, RR 18, SpO2 97%, Temp 36.8
26
(9)
27
Thrombolysis: <4.5 hours of symptom onset
Thrombectomy: <24 hours of symptom onset
Antiplatelets: all patients
Anticoagulation: only if the cause is AF
28
Absolute contraindication Relative contraindication
Intracranial haemorrhage on CT Major surgery or serious non-head trauma in the previous 14 days Neurosurgery, head trauma or stroke in past 3 months Recent lumbar puncture (usually in the past 7 days) History of intracranial haemorrhage History of major haemorrhage within the past 21 days Active internal bleeding Pregnancy Bleeding diathesis HTN >185 mmHg SBP or >110 mmHg DBP
29
History You are working in A&E. You see a 70-year-old man who is brought in by ambulance after his son noticed he was slurring his speech. This started 3 hours ago. On examination, you note he has 3/5 power of both his left upper limb and 4/5 power of his left lower limb. Observations HR 90, BP 155/89 mmHg, RR 18, SpO2 97%, Temp 36.8
30
Risk factor modification
Driving
31
32
Haemorrhagic stroke
33
TIA
7 days
34
Complication DVT Aspiration pneumonia Neurological sequalae
Nutritional support
35
(1)
History A patient is brought in by ambulance. He is drowsy and was witnessed to have a tonic clonic seizure in the street. On examination you notice a significant right sided hemiparesis. He is struggling to maintain his airway but this improves upon a chin lift maneuver.
36
37
38
39
We need your feedback and support! Release new lecture schedules every Saturday New, interactive website coming very soon Want to get involved? Contact us at opportunities@bitemedicine.com to get your information pack Stay up-to-date!
40
1) Lipothymia [CC BY-SA 3.0 (http://creativecommons.org/licenses/by-sa/3.0/)] 2) Circle of Willis. Rhcastilhos [Public domain] https://commons.wikimedia.org/wiki/File:Circle_of_Willis_en.svg 3) mailto:ralf@ark.in-berlin.de / CC BY-SA (https://creativecommons.org/licenses/by-sa/4.0) 4) Miquel Perello Nieto / CC BY-SA (https://creativecommons.org/licenses/by-sa/4.0) 5) OpenStax College / CC BY (https://creativecommons.org/licenses/by/3.0) 6) derivative work: Frank Gaillard (talk)Brain_stem_normal_human.svg: Patrick J. Lynch, medical illustrator / CC BY-SA (https://creativecommons.org/licenses/by-sa/3.0) 7) Dhru4you / Public domain 8) derivative work: Frank Gaillard (talk)Brain_human_sagittal_section.svg: Patrick J. Lynch, medical illustrator / CC BY-SA (https://creativecommons.org/licenses/by-sa/3.0) 9) INFARCT.jpg: Lucien Monfilsderivative work: W2eK / CC BY-SA (https://creativecommons.org/licenses/by-sa/3.0)
All other images are property of BiteMedicine and not to be redistributed