A(H1N1) Influenza Outbreak in Bulgaria and ECDC Mission 44, 45, 46 - - PowerPoint PPT Presentation
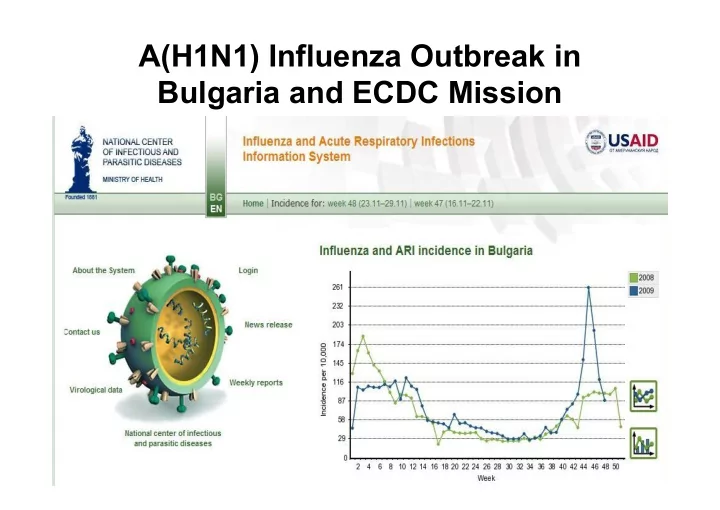
A(H1N1) Influenza Outbreak in Bulgaria and ECDC Mission 44, 45, 46 - - PowerPoint PPT Presentation
A(H1N1) Influenza Outbreak in Bulgaria and ECDC Mission 44, 45, 46 week (26.10-15.11.2009) 44 45 46 AH1N1 RT-PCR tests done in the National Reference Laboratory, May-November, 2009 748 Total number of samples - 2191 Positive for
44, 45, 46 week (26.10-15.11.2009) 44 45 46
AH1N1 RT-PCR tests done in the National Reference Laboratory, May-November, 2009
748
Total number of samples - 2191 Positive for A(H1N1)pdm - 748 (34,1%)
Distribution of samples by age groups
149 370 703 872 97 37 201 279 220 11 100 200 300 400 500 600 700 800 900 1000 0-4г. 5-14г. 15-29г. 30-64г. 65+
Total number of samples Posititve for A(H1N1)pdm
50 100 150 200 250 300 350 400 450 40 41 42 43 44 45 46 47 48
Distribution of samples by week 40 – 48, 2009
.
Total number of samples Positive for A(H1N1)pdm
Distribution of deaths by age groups
34% 34%
66% 6% 11 11 21 21
15-29 15-29 30-64 0-64
cases %
Distribution of deat Distribution of deaths by sex hs by sex
women 44% men 56%
Distribution of deaths by time of seeking medical help
- n
n time ime late ate
cases %
72 2 % 28 % 28 % 23 23 9
20 40 60
Distribution of deaths by antiviral treatment Distribution of deaths by antiviral treatment starting time starting time
- n time
31% late 56% no treatment 13%
Distribution of deaths by presence of risk factors
no risk; 41 pregnancy; 9 chronic illnesses; 38
- besity; 12
Fatal cases EU/EFTA countries Week 50
Fatal cases EU/EFTA countries Week 17
Fatal cases EU/EFTA countries Week 18
Fatal cases EU/EFTA countries Week 19
Fatal cases EU/EFTA countries Week 20
Fatal cases EU/EFTA countries Week 21
Fatal cases EU/EFTA countries Week 22
Fatal cases EU/EFTA countries Week 23
Fatal cases EU/EFTA countries Week 24
Fatal cases EU/EFTA countries Week 25
Fatal cases EU/EFTA countries Week 27
Fatal cases EU/EFTA countries Week 28
Fatal cases EU/EFTA countries Week 29
Fatal cases EU/EFTA countries Week 30
Fatal cases EU/EFTA countries Week 31
Fatal cases EU/EFTA countries Week 32
Fatal cases EU/EFTA countries Week 33
Fatal cases EU/EFTA countries Week 34
Fatal cases EU/EFTA countries Week 35
Fatal cases EU/EFTA countries Week 36
Fatal cases EU/EFTA countries Week 37
Fatal cases EU/EFTA countries Week 38
Fatal cases EU/EFTA countries Week 39
Fatal cases EU/EFTA countries Week 40
Fatal cases EU/EFTA countries Week 41
Fatal cases EU/EFTA countries Week 42
Fatal cases EU/EFTA countries Week 43
Fatal cases EU/EFTA countries Week 44
Fatal cases EU/EFTA countries Week 45
Fatal cases EU/EFTA countries Week 46
Fatal cases EU/EFTA countries Week 47
Fatal cases EU/EFTA countries Week 48
Fatal cases EU/EFTA countries Week 49
Fatal cases EU/EFTA countries Week 50
Purpose of the visit
- to exchange experience regarding pandemic
influenza, as Bulgaria was increasingly affected by the pandemic
- to review and discussion of measures taken to
control the epidemic of pandemic influenza – based on mission check list prepared by ECDC influenza team and
- planning of further actions and cooperation
points
ECDC experts’ conclusions
- The threat to health posed by the A(H1N1) pandemic
influenza virus in Bulgaria does not substantially differ from that in other EU Member States.
- The clinical pattern of disease appeared to be similar
to that in other EU countries, with most affected people only experiencing mild illness. However, a number of people have been very seriously ill.
- Bulgaria is well placed to respond to the 2009
A(H1N1) pandemic, though the plan had to be adapted to respond to the rapidly developing epidemiological situation.
Immediate measures taken by public health authorities in Bulgaria
– activation of national and regional pandemic emergency
- perational units (centres) – daily reporting from regional to the
national level required on the bed capacity and utilization, incidence rates, morbidity pattern and deaths, utilization and availability of antiviral in hospitals. – authoritative information about the pandemic virus was communicated to the public and health professionals - meetings with: hospital directors; directors of regional public health centres, emergency health care units, journalists and other relevant stake holders – clear clinical guidance has been elaborated, adapted and disseminated to different levels of medical care – morning filter in schools and closure of schools for one week – distribution of antivirals to regional centres and hospitals – changes in the legislation to facilitate vaccine and antiviral purchase agreements
Identified strengths of preparedness
- Dedication and high level of expert knowledge of staff of the
Department of Public Health and the National Center of Infectious and Parasitic Diseases working to address the rapidly developing epidemiological situation.
- Availability of comprehensive pandemic plan and rapid
adaptation of the plan to changing epidemiological situation.
- Efforts to increase the AV availability and plans to distribute to
Emergency Care centres.
- Regional communicators were all trained in media relations
prior to the pandemic.
- Combined actions with the ministry of education – introduction
- f daily (morning) health checks and closure of schools.
- Intensive discussions on vaccination policy and plans
- Communication with international organizations (WHO,
ECDC, European commission)
The main suggestions and advice
- f ECDC team for further actions:
- monitoring epidemiological situation in the country for early signs of
possible resurgence and / or possible second wave,
- bserving the number of influenza-related hospitalizations and
deaths which may still be increasing for some period of time while ILI incidence may be going down,
- planning and preparing vaccination campaigns, GPs can be used to
help in identifying persons in risk groups.
- reinforcing the communication to clinicians, especially GPs, and the
public, about the need for early AV treatment (especially for those with underlying conditions predisposing to severe course of infection),
- performing an overall evaluation of the impact of measures applied
for the control of the pandemic may be considered by the Bulgarian PH authorities.
Further actions
- Sharing experiences (ECDC advisory forum – 8
Dec; meeting in Bucharest – 15 Dec)
- Elaboration and adaptation of vaccination plans
– Pandemic vaccination – Seasonal influenza vaccination § Prepare and review plans for resource availability during holidays (X-mas and new year) – staff at central and local levels, primary and specialized health system preparedness – based on planning assumptions of international and local planning assumption § Continuous monitoring of the epidemiological situation
- The great importance of preliminary information from affected countries –
risk groups, clinical manifestation, incidence rate and need for hospitalization, managing severe cases.
- Massive panic among the population, despite the maximum transparency
and openness or namely because of them. The borderline between good information awareness and psychosis is rather thin and easy to cross.
- Need for external expert support – benefit from the reputation of the
specialised international institutions. Nobody can be a prophet in his own land!
- Emergency situations require emergency decisions! This also refers to the
legislation, most of the procedures envisaged are slow and cumbersome and not apt for emergencies.
- No matter how prepared you may be, there will always be things you have
not prepared for. But, there is a positive touch, too – proposals which have been discussed for years are resolved very quickly in a time of crisis. Both the public and the politicians are much more open to health related issues.
Observations and notes
Discussion issues
- Unbalanced contracts for supply of pandemic vaccine. The current
provisions assign plenty of responsibilities to the national authorities and
- nly one right, i.e., the right to pay no matter what. I, personally, would not
sign, nor would I advise the minister to sign under such a contract.
- Long-term consequences of a pandemic. The public has only a certain
amount of threats it can absorb and we are on the verge of exhausting it. This will inevitably cause problems with the future actions to improve the seasonal influenza vaccine coverage, for example, or with the preparedness to face other challenges related to public health.
- Lack of a quick, reliable and effective mechanism for mutual support
among EU member states. Practically, the only real support we received in response to our request for assistance with the supply of antivirals came from Austria and the WHO. Regardless of the long discussions, it has proved impossible to establish a virtual let alone a real community- wide stockpile of antivirals and vaccines. The common European procedure to deliver vaccines to several member states which was being drafted failed as well.